Articles
Read ArticlesEditor's Note: This article is a reprint. It was originally published July 25, 2017.
Dr. Lee Cowden says most people don't die from cancer; they die from the side effects of treatment. While the "war against cancer" is moving toward more personalized and so-called "precision medicine" treatments, the old standby model of "cut, poison and burn," via surgery, chemotherapy and radiation, is still widely used and regarded as the standard of care for many cancer cases.
One of the major problems with chemotherapy is its indiscriminate toxicity, which poisons your body systemically in an attempt to knock out cancer cells. There have long been signs that this model has fatal flaws and may cause more harm than good. In the case of the breast cancer chemotherapy drug Tamoxifen, for instance, patients must trade one risk for another, as while it may reduce breast cancer, it more than doubles women's risk of uterine cancer.1
Serious, sometimes-fatal side effects (or more aptly, simply effects) of chemotherapy are common, as are serious unforeseen effects that may make your cancer prognosis worse instead of better.
Writing in the journal Science Translational Medicine, researchers from the Albert Einstein College of Medicine revealed that giving chemotherapy prior to surgery for breast cancer may promote disease metastasis, or the growth and spread of cancer to other areas of the body.2 This, in turn, greatly increases a woman's risk of dying from the disease.
Chemotherapy May Make Breast Cancer More Aggressive and Likely to Spread
Preoperative chemotherapy, known as neoadjuvant chemotherapy, is often offered to women because it may help shrink tumors, which increases the likelihood that women will receive lumpectomy surgery instead of a full mastectomy. After performing tests on mice and human tissue, however, the researchers found that doing so may increase the likelihood of metastasis by increasing what are known as "tumor microenvironments of metastasis." As Stat News explained:3
"Called 'tumor microenvironments of metastasis,' these on-ramps are sites on blood vessels that special immune cells flock to. If the immune cells hook up with a tumor cell, they usher it into a blood vessel like a Lyft picking up a passenger. Since blood vessels are the highways to distant organs, the result is metastasis, or the spread of cancer to far-flung sites."
When mice with breast cancer or given human breast tumors were given the chemotherapy, it altered the tumor microenvironment in ways that made them more conducive to cancer spread, including, Stat reported:4
- Increasing the number of immune cells that transport cancer cells into blood vessels
- Making blood vessels more permeable to cancer cells
- Making tumor cells more mobile
In mice, chemotherapy treatment doubled the number of cancer cells in the bloodstream and lungs compared to mice that did not receive the treatment. Further, in 20 human patients who received common chemotherapy drugs, the tumor microenvironments also became more favorable to cancer spread. As The Telegraph noted:
"It is thought the toxic medication switches on a repair mechanism in the body which ultimately allows tumors to grow back stronger. It also increases the number of 'doorways' on blood vessels which allow cancer to spread throughout the body."5
Further, researchers wrote in a 2012 Journal of Clinical Oncology editorial, "Unfortunately, neoadjuvant chemotherapy does not seem to improve overall survival, as demonstrated in the National Surgical Adjuvant Breast and Bowel Project (NSABP) B18 trial, among others."6 This means women may be trading a potential increased risk of cancer metastasis for a treatment that doesn't even improve their chances of survival.
It's Been Known for Years That Chemotherapy Can Trigger Tumor Growth
While the news that chemotherapy may encourage cancer spread may sound surprising, it's not a new discovery. In 2012, researchers found chemotherapy for prostate cancer caused DNA damage in healthy cells and caused them to secrete more of a protein called WNT16B, which boosts tumor growth and may encourage cancer cells to develop resistance to treatment.
"WNT16B, when secreted, would interact with nearby tumor cells and cause them to grow, invade and, importantly, resist subsequent therapy," study co-author Dr. Peter Nelson, of the Fred Hutchinson Cancer Research Center, told AFP News.7
In the journal Nature Medicine, the researchers further noted, "The expression of WNT16B in the prostate tumor microenvironment attenuated the effects of cytotoxic chemotherapy in vivo, promoting tumor cell survival and disease progression"8 and "… [D]amage responses in benign cells … may directly contribute to enhanced tumor growth kinetics."9
While research continues to reveal that chemotherapy's effects are wide-reaching and devastating to healthy cells, it's also been shown — at least as far back as 2004 — that "chemotherapy only makes a minor contribution to cancer survival."10 A Clinical Oncology study found that in terms of five-year survival rates in adult cancer cases, chemotherapy has an average five-year survival success rate of just 2.3% in Australia and 2.1% in the U.S.11
Separate research revealed that out of nearly 2,000 patients receiving chemotherapy, 161 deaths occurred within 30 days of the treatment. Nearly 8% of them were classified as related to the chemotherapy (and another nearly 16% were unclassified due to insufficient information).12
Further, as mentioned, chemotherapy can increase the risk of subsequent cancer, such as therapy-related acute myeloid leukemia (tAML), "a rare but highly fatal complication of cytotoxic chemotherapy." Researchers noted that tAML cases occur nearly five times more often in adults treated with chemotherapy than they do in the general population.13
Conventional Oncologists Aren't Likely to Explain the Many Options for Treatment
Upon receiving a cancer diagnosis, many people assume their only options for treatment are chemotherapy, surgery or radiation. Only you and your health care team can make the decision on how to best pursue treatment, but you should know that conventional providers are unlikely to think outside the box.
Oncology is the only specialty in medicine that is allowed and even encouraged to sell drugs at massive profits — typically in excess of 50% — and cancer drugs are, as a general category, the most expensive medications in all of medicine to begin with. Oncologists actually get a commission for the chemotherapy drugs they sell, and with that type of incentive, it's nearly impossible to imagine them actively seeking other alternatives.
Oncologists are further constrained by the "standard of care" prescribed by oncology medical boards and the drug industry. If they go against the established standard of care, they're susceptible to having their license reprimanded or even taken away. As a result, patients are typically forced to go it alone if they don't want to go the conventional route, which is unfortunate because there are many promising alternative treatments.
Understanding Your Options for Cancer Treatment
A comprehensive natural cancer-fighting approach would be to make your body as healthy as possible, using detoxification, strategies to boost your immune function, dietary changes and other targeted therapies depending on your needs. For instance, Annie Brandt — a 16-year cancer survivor and author of "The Healing Platform: Build Your Own Cure!" — states products that are helpful against metastatic cancer cells include:
Berberine / metformin |
Intravenous vitamin C |
Sulforaphane (cruciferous vegetables) |
Curcumin (turmeric) |
Broccoli sprouts |
Glucoraphanin |
Myrosinase |
Essiac tea |
Burdock root |
Slippery elm |
Rhubarb |
Sheep sorrel |
Fermented soy |
Fish oil |
Modified citrus pectin (PectaSol-C) |
Heparin |
The point is that there are many anticancer strategies overlooked by conventional medicine. Many of them even work in addition to conventional treatment. For instance, vitamin C in combination with nutritional ketosis and fasting prior to administering chemotherapy radically improve the effectiveness of chemotherapy.
Oncologists in Turkey, who aren't under the same U.S. restrictions, are also using a stacked ketogenic treatment protocol that is showing shocking remissions in many stage 4 cancer patients. The treatment protocol at ChemoThermia Oncology Center in Turkey includes:
- Metabolically supported chemotherapy (applying chemotherapy with a variety of interventions to support its effectiveness)
- Hyperthermia
- Hyperbaric oxygen therapy
- Glycolysis inhibitors, especially 2-deoxyglucose (2-DG) and dichloroacetate (DCA)
- Ketogenic diet with phytopharmaceutical supplements
At the center, all oncology patients are put on a ketogenic diet, which creates metabolic stress on the cancer cells. Then, prior to administering the chemo, the patient will do a 14-hour fast, which further increases the metabolic stress on the cancer cells.
The patients will typically have a blood glucose level around 80 milligrams per deciliter (mg/dL) at this point. They then apply glycolysis inhibitors to inhibit the glycolysis pathway in the cancer cells, which creates a terrific amount of metabolic stress, as the cancer cells are already starved of glucose.
Insulin is then applied to lower the blood glucose levels to around 50 or 60 mg/dL, to cause mild hypoglycemia. At that point, chemotherapy is applied, often at a far lower dose than would otherwise be used, thereby lowering the risk of side effects.
In the days following chemotherapy, hyperthermia and hyperbaric oxygen therapy are applied, plus a daily infusion of glycolysis inhibitor therapies with high-dose vitamin C (50 grams) and dimethyl sulfoxide (DMSO). A sampling of other targeted therapies covered in Brandt's book are below.
Poly-MVA, a colloidal mineral complex that crosses the blood-brain barrier and helps renourish your body and brain at the cellular level. It also helps replace nutrients lost during chemotherapeutic and radiological treatments. |
AvéULTRA (Metatrol), a fermented wheat germ product. |
Selenium, vitamin D and iodine, as most cancer patients are low in these three nutrients. Since I do regular sauna therapy, I take 200 micrograms of SelenoExcell each day. (You tend to excrete selenium when sweating.) Selenium increases glutathione, an important metabolic antioxidant necessary for detoxification. It also catalyzes the conversion of thyroid hormone T4 to T3, so it can be beneficial if you have thyroid problems. |
Modified citrus pectin (MCP) has been shown to reverse cancer and stop metastatic cancer. Brandt recommends the brand ecoNugenics, as this is the one that has been scientifically studied and verified to work. |
Colloidal silver is a nontoxic, broad-spectrum antimicrobial therapy with no known toxicity and no known mechanism for acquired resistance. |
Salicinium, a plant-based extract that inhibits production of nagalase — an enzyme produced by cancer cells — while simultaneously stimulating innate immune cells. |
So as mentioned, there are many promising avenues to target cancer. Even if you're working with a conventional oncologist, the ChemoThermia Oncology Center has published protocols your oncologist could make use of, regardless of where you live. If your oncologist isn't willing to integrate these alternative strategies into your care regimen, you may want to consider finding a new doctor.
Chemotherapy Spreading Cancer
Take a look at the length of your index finger and your ring finger. Is your ring finger longer? If so, it could be a sign of psychopathic tendencies and antisocial personality traits.1 This is because the index finger-to-ring finger ratio (2D-to-4D ratio) is linked to exposure to hormones, specifically testosterone and estrogen, in the womb.
These exposures may have a lasting effect on human health and behavior, it turns out. A lower 2D-to-4D ratio — meaning the ring finger is longer than the index finger — is associated with higher testosterone exposure and lower estrogen exposure in the womb during the first trimester. It also signals an increased likelihood of certain psychiatric disorders, according to research published in the Journal of Psychiatric Research.2
Digit Ratios May Predict Eating Disorders, Personalities, Obesity and More
Digit ratios, particularly the 2D-to-4D ratio, is widely considered a proxy for prenatal sex hormone exposure. As such, there are noted differences between men and women, with males, who are exposed to more testosterone, typically having lower ratios than females.
Further, in men a lower 2D-to-4D ratio is linked with physical aggression and enhanced sports performance,3 while lower digit ratios are also associated with being left-handed, an increased risk for anxiety and, in females, assertiveness. But the tendency for digit ratio to predict behavior and health status goes even further, as digit ratios, whether low or high, are associated with:4
Numerical competencies |
Spatial skills |
Handedness |
Cognitive abilities |
Academic performance |
Sperm counts |
Personalities |
Obesity |
Migraine |
Eating disorders |
Depression |
Myopia |
Autism |
"The topic is interesting, because the relation of the lengths of index finger (2D) and ring finger (4D) is one of the most robust biological markers formed during the prenatal stage with a remarkable impact later on an adult's behavior," Serge Brand of the University of Basel and Kermanshah University of Medical Sciences told PsyPost, adding:5
"More specifically, a lower 2D:4D-ratio, that is to say, that the index finger is shorter compared to the ring finger, is strongly associated with an increased exposure to testosterone and with a decreased exposure to estrogen during the prenatal stage.
Now, several original studies, meta-analyses and systematic reviews showed that a lower 2D:4D-ratio as a proxy of prenatal sex steroid exposure enables an adult organism to outperform in behavior in case of necessity.
What was unclear so far was, if such sex steroid exposure during the prenatal stage might be mirrored in an adult's behavior such as amphetamine use disorder and antisocial personality disorder."
Brand and colleagues conducted a study to find out, assessing whether 2D:4D ratios differed among people with amphetamine use disorder (AUD) and antisocial personality disorder (ASPD), which involves manipulative, impulsive and often criminal behavior.
People With Psychiatric Conditions Have Lower 2D-to-4D Ratios
To calculate digit ratio, the length of the index finger (2D) is divided by the length of the ring finger (4D). A ring finger that's longer than the index finger, which leads to a lower digit ratio, suggests higher exposure to testosterone in the womb.
The study involved 44 people with AUD, ASPD or both AUD and ASPD, along with 36 healthy controls. Those with the psychiatric conditions had significantly lower 2D-to-4D ratios compared to those without. Further, those with both AUD and ASPD had the lowest 2D-to-4D ratios. Having a lower 2D-to-4D ratio was also linked with higher 'Dark Triad' (DT) traits, which involve narcissism, Machiavellianism and psychopathy. According to the study:6
"The lower the 2D:4D-ratio, the higher the DT scores among the clinical sample. In our opinion, this finding is of greater importance, in that DT traits were associated with various types of negative psychosocial and psychological outcomes, including IU [intolerance of uncertainty], callous affect and interpersonal manipulation.
Given this, it appears that DT traits could be biologically rooted in higher testosterone and lower estrogen concentrations during the fetal phase of the first trimester."
Even the researchers were surprised to see such a strong association between greater psychopathology symptoms and a longer ring finger compared to the index finger. Brand told PsyPost:7
"We were surprised to observe such a linear association between higher symptoms of psychopathology and lower 2D:4D-ratios. That is to say: The more an adult participant had signs of psychopathology, the more it appeared that this adult has been exposed to higher testosterone concentrations and lower estrogen concentrations during the prenatal period of life."
He also pointed out, however, that finger length alone doesn't dictate the state of your mental health and, in some cases, a lower 2D-to-4D ratio could be beneficial, such as in competitive sports:8
"It is important to understand that the finger lengths-ratio as a proxy of a specific exposure to prenatal sex steroids should not be understood as a person's irrevocable fate! Rather, a lower 2D-to-4D ratio and thus a higher exposure to testosterone during the prenatal period of physiological development might enable an adult person to show a specific pattern of behavior.
To make the case in point, compared to 117 age- and sex-matched sedentary females, 104 Swedish female Olympic athletes had statistically significantly lower 2D-to-4D ratios9 or, simply put: The Swedish female Olympic athletes were exposed to higher testosterone and lower estrogen concentrations during their prenatal stage of development."
Psychiatric Patients Tend to Have Longer Ring Fingers Than Index Fingers
A systematic review of case-control studies similarly found that psychiatric patients had lower 2D-to-4D ratios than people without psychiatric disorders.10 In the case of autism spectrum disorder, attention deficit hyperactivity disorder (ADHD) and addictions, 2D:4D ratio was significantly lower than in those without the conditions. The researchers noted:11
"Our finding is important because, on one hand, it may propose 2D:4D as a potential biomarker for psychiatric disorders in general; on the other hand, it highlights the role of prenatal exposure to hormones, specifically testosterone, in the etiopathogenesis of psychiatric disorders."
Beyond mental health, 2D:4D ratio has also been linked with "a wide number of traits and conditions, ranging in almost every field of medicine," the study explained, including conditions dependent on sex hormones as well as physical characteristics and behaviors. Examples include:12
Breast cancer |
Prostate cancer |
Osteoarthritis |
Facial shape |
Age of menarche |
Penis size |
Stuttering |
Visuo-spatial ability |
Schizotypal personality |
Sporting ability |
Successful financial risk-taking |
Sexual orientation |
Men With Long Ring Fingers May Experience Mild COVID-19
Digit ratio may also be a strong indicator of men's vulnerability to COVID-19, due to its relation to testosterone exposure in utero. Higher testosterone levels are deemed protective due to their effects on the angiotensin-converting enzyme 2 (ACE2). Researchers at the U.K.'s Swansea University measured the ring fingers of 103,482 men and 83,366 women from 41 countries in relation to their index fingers.13
In countries with a smaller digit ratio (0.976 millimeters (mm)), such as Malaysia, Russia and Mexico, COVID-19 fatality rates were lower than in countries with a higher digit ratio (0.99 mm and greater, which indicates a shorter ring finger), such as the U.K., Spain and Bulgaria.14 Overall, men in countries with longer ring fingers had a COVID-19 death rate of 2.7 per 100,000, compared to 4.9 per 100,000 in countries with a shorter overall ring finger length.15
"Our findings support a link between high 2-to-4D (low prenatal testosterone) and high severity of COVID-19 in men," the researchers explained, adding, "Thus, high prenatal testosterone (low 2D-to-4D) in men may be protective of the serious effects of COVID-19 … A strong positive association between male 2D-to-4D and mortality may provide a biomarker for male COVID-19 susceptibility …"16
One theory for why men with shorter ring fingers have a higher risk of severe outcomes from COVID-19 has to do with ACE2, an enzyme that's beneficial in that it promotes tissue regeneration. The problem is that coronavirus binds to ACE2 and uses it to enter cells,17 where it then multiplies. But when levels rise high enough, ACE2 may actually be protective.
Professor John Manning, lead researcher of the study, noted, "The theory is that someone with high prenatal testosterone — and a long ring finger — has greater levels of ACE2. These concentrations are large enough to oppose the virus … Our findings may be men with long ring fingers will experience mild symptoms and could return to work."18 Writing in Early Human Development,19 the researchers further explained the paradox:
"SARS-CoV2 enters cells via the receptor molecule ACE2. Paradoxically, the up-regulation of ACE2 relates to protective effects from COVID-19 infection, possibly because it opposes the loss of ACE2 from cell surfaces. We speculate that in men the up-regulation of ACE2 relates to high testosterone and low 2D:4D."
How to Support Positive Mental Health
While you can't choose or change your 2D-to-4D ratio — and it remains constant throughout life20 — it's not the only measure of your mental health. Further, there's plenty you can do to support optimal psychological well-being. Getting optimal exposure to sunlight daily and regular physical activity, particularly three to five days a week for 45 minutes,21 can improve mental health.
You can also use the Emotional Freedom Techniques (EFT) or the Neuro-Emotional Technique's First Aid Stress Tool, or NET FAST,22 to help relieve stress. Here is a summary of the FAST procedure:
- While thinking about an issue that is bothering you, place your right wrist, palm up, into your left hand. Place three fingers of your left hand onto the area of your right wrist where you can feel your pulse.
- Place your open right hand on your forehead. Gently breathe in and out several times while concentrating on feeling the issue that bothers you.
- Switch hands and repeat steps 1 and 2.
Getting a sound night's sleep is also important, as too little sleep may increase anxiety by up to 30%,23 while deep sleep was shown to have anxiety-relieving effects. If you're struggling with anxiety, making sleep a priority may calm your brain and your mind, helping to resolve anxiety symptoms.
Further, the more sleep deprived you are, the less social you become, and others pick up on this largely subconscious cue to be left alone, essentially turning people into "social lepers" and fueling an epidemic of loneliness.24 A short temper and unwanted behaviors such as rudeness can also be the result of a poor night's rest.25
Eating healthy is another key. Researchers from Macquarie University, Australia, studied 76 students between the ages of 17 and 35 who followed a poor diet and had moderate to high levels of depression symptoms.26,27
One group of participants was asked to improve their diet by cutting back on refined carbohydrates, sugar, processed meats and soft drinks, while eating more vegetables, fruits, dairy products, healthy fats and anti-inflammatory spices such as turmeric and cinnamon.28 After only three weeks of healthier eating, those in the healthy diet group had significant improvements in mood and their depression scores went into the normal range.
In addition to 2D-to-4D ratio, researchers are also exploring whether other prenatal factors influence personality and behavior later in life.29 No matter the cause, if you're experiencing a serious mental health problem, always seek the guidance of an integrative health practitioner who can help you get started on your healing journey. If you're in the midst of a mental health crisis, get emergency medical care.
Does Your Finger Length Reveal Psychopathic Tendencies?
In addition to the weather modification1 going on around the world, militaries around the world are also routinely dispersing tiny bits of aluminum-coated fiberglass and plastic — known as “chaff” — into the air column, to shield aircraft and ships from enemy radar.2 Not surprisingly, this has been done for decades, without clear evidence that it’s safe for humans and the environment.
According to a 1998 General Accounting Office report3 and a 1999 follow-up report4 by the Naval Research Laboratory, the environmental, human and agricultural impacts of chaff used in military training scenarios at the time were “negligible and far less than those from other man-made emissions,” but does that really mean it’s safe? As explained in a 2001 Navy Medicine paper:5
“Radiofrequency (RF) chaff is an electronic countermeasure designed to reflect radar waves and obscure planes, ships, and other assets from radar tracking sources.
Chaff consists of aluminum-coated glass fibers (also referred to as dipoles) ranging in lengths from 0.8 to 0.75 cm. Chaff is released or dispensed from military vehicles in cartridges or projectiles that contain millions of dipoles.
When deployed, a diffuse cloud of dipoles is formed that is undetectable to the human eye. Chaff is a very light material that can remain suspended in air anywhere from 10 minutes to 10 hours and can travel considerable distances from its release point, depending on prevailing atmospheric conditions.
Training for military personnel, particularly aircraft pilots, in the use of chaff is necessary to deploy this electronic countermeasure effectively. As with most acquired skills, the deployment of chaff must be maintained by practicing in-flight release during training.
It is estimated that the U.S. Armed Forces dispense about 500 tons of chaff per year, with most chaff being released during training exercises within the continental United States.”
Is Chaff Safe?
According to the Naval Medicine investigation, inhalation of whole, intact chaff fibers pose “no risk” to humans due to their larger size. “If inhaled, dipoles are predicted to deposit in the nose, mouth, or trachea and are either swallowed or expelled,” the paper states.6
Note the use of the word “predicted,” however. Predictions are not evidence. They’re basically guessing. Open questions also remain about what happens when the fibers degrade.
“Several investigations have demonstrated that Al-coated dipoles are resistant to weathering and breakdown under desert conditions,” the paper states.7
“A 1977 US Navy-sponsored a study found no evidence to indicate that chaff degrades significantly or quickly in water from the Chesapeake Bay nor did this material leach significant amounts of aluminum into the Bay.
A recent study by our group found no evidence that 25 years of chaff operations at the Naval Research Laboratory detachment at Chesapeake Beach, MD resulted in a significant increase in sediment or soil aluminum concentrations (Wilson et al 2000).
However, additional studies are needed to determine the half-life of chaff dipoles in various soils and environmental conditions and whether dipoles breakdown to respirable particles ...
Although there is no definitive evidence from the epidemiological literature that chaff exposure is not harmful, there is epidemiological information available on workers involved in the glass fiber manufacturing industry. Data from these studies suggests that exposure to fibrous glass is not associated with increased risk of death from respiratory disease.”
The problem with that is that fiberglass workers are equipped with protective gear, including respirators, Tyvek suits and safety goggles8 — gear that normal people don’t wear when they’re out and about. All this tells us is that chaff is unlikely to cause harm to public health, provided people are wearing respirators, which they don’t.
Remarkably, not much beyond these three reports exist. While all admitted the need for continued research, none appears to have been published, so there’s really no telling what the real-world impact might be. That said, common sense tells us that air dispersed aluminum and fiberglass is highly likely to have some sort of impact on the environment and human health.
Geoengineering Has Been Going on for Decades
Aluminum and fiberglass are not the only toxins being sprayed across our skies. As detailed by Dane Wigington, founder of Geoengineeringwatch.org, weather modification, also known as geoengineering, in which various toxic metals and chemicals are dispersed at high altitude, has been going on for more than 70 years, and is increasing rather than declining.
In response to a United Nations Intergovernmental Panel on Climate Change (IPCC) report issued in August 2021,9,10 which called for radical measures to prevent further global warming, the Biden Administration launched a research effort in 2022 to determine the most effective way to dim the sun.11
One proposal involves injecting sulfur dioxide aerosols into the Earth's stratosphere. The tiny reflective particles would bounce sunlight back into space instead of onto the Earth’s surface.12 According to Harvard researchers,13 this strategy is not only “technically possible” but also “remarkably inexpensive,” having a price tag that is “well within the reach of several nations.”
Earth’s climate is largely controlled by how much solar radiation reaches the Earth and how much is absorbed by its surface or reradiated to space. Cloud coverage and greenhouse gasses are examples of factors that influence the reflectance of solar radiation.14
“If geoengineering proposals are to influence global climate in any meaningful way, they must intentionally alter the relative influence of one of these controlling mechanisms,” Britannica explains.15
The U.N. report mentions solar radiation management and greenhouse gas removal as forms of geoengineering.16 Sulfate aerosols fall into the solar radiation management category. By reflecting more solar radiation back into space, the aerosols lower global temperatures but also have a serious “side effect” — they lower average precipitation.
As a result, additional geoengineering techniques — such as thinning out cirrus clouds in the upper atmosphere — would be necessary to counteract the decrease in precipitation. What could possibly go wrong?
Supercomputers have run models to predict how solar radiation management may affect different parts of the Earth, not only in terms of temperature but also rainfall and snowfall. Report author Govindasamy Bala, from the Indian Institute of Science, said “the science is there,”17 but it’s far from an exact one.
“I think the next big question,” Bala told Reuters, “is, do you want to do it? ... That involves uncertainty, moral issues, ethical issues and governance.” As Reuters reported, “That's because every region would be affected differently. While some regions could gain in an artificially cooler world, others could suffer by, for example, no longer having conditions to grow crops.”18
‘Catastrophic Risks’
Three months after the IPCC published its panic-inciting report, Australian and British researchers published an original research article warning that stratospheric aerosol injection carries “catastrophic risks” that may well lead us into “a fate worse than [global] warming”:19
“Injecting particles into atmosphere to reflect sunlight, stratospheric aerosol injection (SAI), represents a potential technological solution to the threat of climate change. But could the cure be worse than the disease? ...
SAI plausibly interacts with other catastrophic calamities, most notably by potentially exacerbating the impacts of nuclear war or an extreme space weather event. SAI could contribute to systemic risk by introducing stressors into critical systems such as agriculture.
SAI's systemic stressors, and risks of systemic cascades and synchronous failures, are highly understudied. SAI deployment more tightly couples different ecological, economic, and political systems. This creates a precarious condition of latent risk, the largest cause for concern ...
A well-coordinated use of a small amount of SAI would incur negligible risks, but this is an optimistic scenario. Conversely, larger use of SAI used in an uncoordinated manner poses many potential dangers. We cannot equivocally determine whether SAI will be worse than warming. For now, a heavy reliance on SAI seems an imprudent policy response.”
In June 2023, the European Commission put out a call for “international talks on the dangers and governance of geoengineering,” warning that geoengineering schemes aimed at altering the global climate pose “unacceptable” risks. During a news conference, EU climate policy chief Frans Timmermans stated:
“Nobody should be conducting experiments alone with our shared planet. This should be discussed in the right forum, at the highest international level.”
Time will tell whether such talks ever take place. In September 2023, the Climate Overshoot Commission, chaired by Pascal Lamy, a former World Trade Organization chief, called for a worldwide moratorium on solar radiation modification experiments “that would carry risk of significant transboundary harm,” and to focus instead on strategies to reduce greenhouse gas emissions.20,21 But, as of yet, no such moratorium has been agreed upon.
Socialist Ideology, Not Climate Science
Zuzana Janosova Den Boer experienced Communist rule in Czechoslovakia before moving to Canada. In her article, “I Survived Communism — Are You Ready for Your Turn?” she detailed the “all-too familiar signs of the same propaganda” starting to permeate her adopted country.22
In relation to geoengineering, she points out that communism has been subverting the environmentalist movement since the 1970s, when then-chairman of the Communist Party USA, Gus Hall, published a book called “Ecology,” in which he stated:23
“Human society cannot basically stop the destruction of the environment under capitalism. Socialism is the only structure that makes it possible … We must be the organizers, the leaders of these movements.”
Den Boer writes:24
“This idea was incorporated into the U.S. Green Party program in 1989 ... in which the fictitious threats of ‘global warming’ and ‘climate change’ are used to scare the public into believing humanity must ‘save the planet’:
‘This urgency, along with other Green issues and themes it interrelates, makes confronting the greenhouse [effect] a powerful organizing tool … Survival is highly motivating, and may help us to build a mass movement that will lead to large-scale political and societal change in a very short time …
First of all, we [must] inform the public that the crisis is more immediate and severe than [they] are being told, [that] its implications are too great to wait for the universal scientific confirmation that only eco-catastrophe would establish.’”
The U.N.’s Intergovernmental Panel on Climate Change (IPCC), Den Boer suggests, is promoting not climate science but socialist ideology, citing as evidence comments made by Ottmar Georg Edenhofer, former co-chair of the IPCC Working Group III, who in a 2010 interview stated that climate issues are about economics, and that:25
“We must free ourselves from the illusion that international climate policy is environmental policy … We must state clearly that we use climate policy de facto to redistribute the world’s wealth.”
Geoengineering Poses Extinction-Level Threat to Humanity
Even without factoring in social control, the practical risks of geoengineering are impossible to ignore. According to scientific studies, the particulates dispersed during these geoengineering events “shred” the ozone layer. They also disrupt the hydrological (rain) cycle, which leads to another host of downstream effects, and this is in addition to spreading toxins across the entire planet surface.
So, while some of the planet might benefit from these programs, other parts could be decimated by droughts, raging forest fires, flooding or storms. Moreover, while global cooling is the stated aim of most of these geoengineering programs, as the planet warms, the laws of physics state you need more precipitation to cool it, not less, because the atmosphere carries more moisture as the temperature rises.
To cool the planet, you need to create more rain, but these programs have resulted in less rain, and the reason for the reduction in rain fall is due to the particulates in the atmosphere. In addition to deflecting heat from the outside, these particles also trap heat down below, making the overall heating of the planet massively worse.
The risks are so immense, Wigington warns geoengineering already poses an extinction-level threat to humanity. The window of opportunity to save ourselves is rapidly closing.
Unfortunately, if people really understood the totality of the situation — not just that the climate is being manipulated, but that as a result, the global climate systems have deteriorated to the point that the entire Earth is in serious trouble; in short, that these programs may have created a runaway extinction event — the emotional impact might be too great to bear for many. Wigington addressed this in an interview I did with him back in 2016:
“Our situation is far more severe than most people have any understanding of,” he said. “Climate engineering is making the situation worse, not better.
So [they must] try to keep the population from panicking because of the severity and immediacy of the climate implosion, and keep the population in the dark because the climate intervention programs have helped to accelerate this process and toxified every single one of us in the process.
Every single human subject we test is packed full of aluminum, barium — all the heavy metals we know are associated with these programs. It doesn’t matter where they live.
And we know it’s coming down in the precipitation in unimaginable quantities — quantities enough to change soil pH values in the Pacific Northwest 10 to 12 times total alkaline — that’s an unimaginable amount of metal coming down in the rain.
If populations understood, truly, what’s been done to them, what’s been done to the planet … they’d be taking to the streets with pitchforks and torches all over the globe.”
California Aquatic and Terrestrial Insect Life Has Been Decimated
Geoengineeringwatch.org lists a number of lab tests that have been performed on rain water, air sample and more, and their results. You can find them under the Tests section.
“In regard to the effect in the environment, in Northern California alone … what we’ve seen in the last decade … is a 90% decline in aquatic and terrestrial insect life — a virtual crash,” Wigington told me in 2016.
“There’s so much aluminum coming down the precipitation, affecting the soil pH, and — this is very important — the UV radiation level is off the charts, and that we can link directly to climate engineering … We’re seeing UVB levels about 1,000% higher than we’re being told. It’s burning the bark off of trees. It’s killing plankton. It’s affecting insect life …
[It increases UVB radiation] because it shreds the natural protection for the planet. When you put a particle in the atmosphere, it doesn’t matter whether it’s from a back of a jet or a volcano; it causes a chemical reaction in the atmosphere that destroys ozone. Period. So the more of these particles you put in the atmosphere, the more rapid the ozone destruction is.”
With all of that in mind, it’s highly unlikely that military chaff dispersements have no negative impact. An argument could be made that chaff is too important of a defense system to get rid of, and that may be true. But the climate-specific engineering is another matter altogether.
In years past, it was kept hush-hush, and dismissed as a conspiracy theory. Since then, however, governments around the world, and international bodies like the U.N. have become quite open about the use of geoengineering for climate control, and if the global public does not push back against these efforts, we might not survive to regret it.
Geoengineeringwatch.org has a list of action items you can review if you want to get involved and get the word out. I also recommend watching Wigington’s documentary “The Dimming,” below, to learn more.
The Military Routinely Disperses Aluminum-Coated Fiberglass Into the Air
There are 55 poison control centers located across the U.S.1 Each day trained experts are connected to the public and professionals who are seeking help or treatment advice. The poison control centers collect this data in real-time, which was the basis of a study from the Abigail Wexner Research Institute in which they analyzed the number, severity and rate of exposure to children, teens and adults to liquid laundry detergent packets.2
Since 1946,3 Tide laundry detergent, manufactured by Procter & Gamble (P&G), has been a part of American culture. Tide introduced the first heavy-duty liquid laundry detergent in 1946 and the formula did not change again until 1968 when enzymes were added to help break down stains.
By 1970, color-safe oxygen bleach was added to the formula to whiten and brighten your clothes. CNN reports4 that in 2004, P&G was looking for a new hit in the consumer market. It had been decades since Tide introduced liquid detergent and cheaper products were encroaching on the brand’s market. The company's next goal was to disrupt "sleepwashing," a term they used to describe consumers who picked up any bottle of detergent on the shelves.
After eight years of trial and error, P&G introduced Tide Pods and it quickly became a breakthrough success. The small, easily transported pods meant consumers didn't have to lug around bulky detergent bottles and didn't have to clean up after spills. But consequences quickly followed. The study investigators identified increases and declines in exposures to children, teens and adults.5
Number of Poisons From Liquid Laundry Detergent Packets Rising
In a study published in Clinical Toxicology, researchers looked at the number of calls related to liquid laundry detergent packets since the 2010s.6 They sought to assess the longitudinal trends in exposure by age, and found poison control centers had recorded 114,826 exposures to single or polysubstance liquid laundry detergent packets from 2014 to 2022.
While the number of calls on children under age 6 increased yearly at first, they declined over the years 2020 to 2022. Researchers attribute this to both public awareness and voluntary product safety changes made by the detergent companies. Overall, though, the under-age 6 group continued to be the most exposed, accounting for 86.8% of all phone calls during the study’s eight years.
When looking at multiyear trends, they found that the same age group had an increased exposure of 16.8% from 2018 to 2020. But that exposure rate declined by 6.8% from 2020 to 2022, during the pandemic and lockdowns. Conversely, the annual exposure rate in adults from 2014 to 2022 rose by 147.1% and in adolescents, rose by 85.4% from 2014 to 2017 and again by 155.3% from 2017 to 2018.
Of all exposures, the most serious medical outcomes and hospitalizations were experienced by children less than age 6. The researchers concluded, "Additionally, exposures have increased among older children, adolescents and adults. Renewed safety efforts are warranted to protect prior public health gains and further reduce exposures."
Newswise7 notes that according to past research, the American Society for Testing and Materials, now ASTM International, published a voluntary standard in 2015. The operative word in the statement being "voluntary." Recent updates were made in March 2022, but those did not substantially change the scope of the standard.
"The voluntary standard, public awareness campaigns, and product and packaging changes to-date have improved the safety of these products, but a high number of children are still exposed each year," said Dr. Christopher Gaw, senior author of the study and emergency medicine physician. "There is still room for improvement."
Liquid Laundry Packets More Toxic Than Other Detergents
The higher toxicity associated with liquid laundry detergent packets as compared to traditional liquid or powder detergents is not well understood.8 Reformulating the products may reduce the severity of the consequences of exposure, but more is required to educate the public about the toxicity of highly concentrated packets.
Gary Smith, co-author of the study and director of the Center for Injury Research and Policy, explains that the voluntary safety standards allow manufacturers to use six different ways to meet the requirement for child-resistant containers rather than conforming to the 1970 Poison Prevention Packaging Act (PPPA), which has been highly effective in preventing unintentional poisoning.
"Requiring that all liquid laundry detergent packet packaging be PPPA-compliant would be an important next step in reducing child access to these products," he said. "In addition, each laundry packet should be individually wrapped with child-resistant packaging, which would provide important layers of protection for this highly toxic product."9
Laundry Pod Exposure Exacerbated by the Tide Pod ‘Challenge’
Tide Pods were developed with the combined efforts of more than 75 employees and 450 product sketches and packaging. Thousands of consumers weighed in with their opinions. P&G launched Tide Pods during the 2012 Academy of Awards, encouraging consumers to "pop" Tide Pods in the machine and watch their clothes brighten with a "pop."10
The lightweight design, colorful swirl, and squishy feel were an instant hit with consumers, propelling sales to $500 million in one year and garnering the company 75% of the single-dose laundry packet market. In addition to the look of the product, people also appear to like the way they feel in their hands.
According to Dr. Frédéric Basso, a professor at The London School of Economics and Political Science, Tide Pods took advantage of a trend in marketing known as "food imitating products."11
By creating a visual or emotive link to food or other positive experiences, the manufacturers hoped that consumers would not associate doing laundry with an unpleasant or boring chore. However, there were consequences. Within two months, there were nearly 250 young children who had eaten the pods, prompting P&G to change the packaging and the container.12
In 2012, the New York Daily News called for the Consumer Product Safety Commission to crack down on detergent company pods that looked more like candy. New York Sen. Charles Schumer commented, "These pods were supposed to make household chores easier, not tempt our children to swallow harmful chemicals. I saw one on my staffer's desk and I wanted to eat it."13
Schumer noted that the pods had been on the market in Europe for several years at that point, where they had also caused serious injuries. He didn't think the products should be banned but "I don’t know why they make them look so delicious," he said.14 Tide Pods then became an internet sensation, propelled by the Tide Pod "Challenge" that encouraged children and teens to eat the detergent pods.
As demonstrated in this video, ingestion has dire consequences for anyone who is enticed by the look and feel of the laundry detergent pods, or foolishly believes that consuming them as a part of a challenge will not harm their health. As explained in the video, detergents are either highly alkaline or highly acidic, both of which cause devastating damage to any tissue it touches, including the mouth, esophagus and trachea.
Potential Effects From Chemicals in ‘Fragrance’
However, it isn’t just the pH of the product that causes damage, but also the chemicals added to the detergents for fragrance and smell. Many laundry detergents base their ad campaigns on the ability of their products to keep your clothes fragrant for days or weeks after washing. This characteristic of detergent is valued by some consumers to the point that magazines publish analyses of how well each smells and for how long.15
Yet, while the chemical combinations in the ingredient "fragrance" are toxic to your senses, they are protected as "trade secrets." According to the FDA, the cosmetics market must reveal their ingredients in the label under the Fair Packaging and Labeling Act, but according to the regulation, the list cannot be forced from the company to disclose "trade secrets."16
"For example, fragrance and flavor ingredients do not need to be listed individually on cosmetic labels, because they are the ingredients most likely to be 'trade secrets.' Instead, they may be listed simply as 'fragrance' or 'flavor.'"
As I have shared in the past, one artificial fragrance can contain dozens of potentially toxic chemicals. When you consider that the industry has 3,100 stock chemical ingredients for their fragrances, you literally could be exposed to thousands of these chemicals every day.
Research by Anne Steinemann, formerly with the University of Washington and currently a professor of civil engineering at the University of Melbourne, Australia, and colleagues tested 25 household products, including air fresheners and all-purpose cleaners, many of them "top sellers" in their category. The team found the average number of volatile organic compounds (VOCs) emitted was 17. They wrote in the journal Environmental Health Perspectives:17
"A single fragrance in a product can contain a mixture of hundreds of chemicals, some of which (e.g., limonene, a citrus scent) react with ozone in ambient air to form dangerous secondary pollutants, including formaldehyde. The researchers detected 133 different VOCs. Most commonly detected were limonene, α- and β-pinene (pine scents), and ethanol and acetone (often used as carriers for fragrance chemicals).
Each product emitted [one to eight] toxic or hazardous chemicals, and close to half (44 percent) generated at least 1 of 24 carcinogenic hazardous air pollutants, such as acetaldehyde, 1,4-dioxane, formaldehyde or methylene chloride. These hazardous air pollutants have no safe exposure level, according to the U.S. Environmental Protection Agency."
You can't tell what types of toxic chemicals might be lurking in your favorite cleaning supplies because such labeling is not required. Fragranced products, which include many commercial cleaning and laundry products, are particularly problematic. Another of Steinemann’s studies18 revealed that 34.7% of Americans reported health problems, such as migraine headaches and respiratory difficulties when exposed to them.
Reduce Exposure Risk Using Nontoxic Cleaners
When you clean your home with commercial sprays, wipes, scrubs and polishes, you're putting toxins into your home environment instead of removing them. The same goes for most laundry detergents, dryer sheets and air fresheners. Even those strong-smelling lemon and pine scents — the ones many people think are the epitome of a clean home — are created by toxic volatile organic compounds (VOCs).
I offer many examples of how you can keep a clean home with nontoxic cleaners, including disinfecting, glass cleaning, dusting and furniture polish. For how to make these cleaners with what you may already have in your home, check out the article. There are also ways you can clean your laundry without sacrificing scent or cleanliness and without using store-bought chemicals.
Castile soap is natural, biodegradable and chemical-free, plus incredibly versatile (as are most natural cleaning supplies). You can use it for personal care, laundry and cleaning around your home. For instance, mixing baking soda with a small amount of liquid castile soap makes an excellent paste for cleaning your tub and shower.
You can easily freshen your laundry without risking your family's health by simply spritzing your wet laundry with a mix of water and a few drops of essential oil before placing it in the dryer. Alternatively, add roughly one dozen drops to an old wool sock, and put it in the dryer with your laundry.
You can even make your own laundry detergent, adding in any essential oils you like for a natural scent. Here's a recipe from Mommypotamus to get you started.19
Homemade Natural Laundry Detergent
Ingredients
- 6 cups washing soda
- 3 bars coconut oil soap (4.5 to 5 ounces each)
- Lemon essential oil (optional)
To Make
- Cut soap into small chunks. Add to a food processor along with the washing soda.
- Blend until you have a fine powder. You may want to lay a dish towel over the top of your food processor to prevent a fine mist of powder from floating into the air. Also, let it settle a bit before opening the container or the powder will float onto your kitchen counter!
- Pour into a clean container (keep the essential oil next to the jar and add five drops with each load).
Poison Centers Received One Call Every 44 Minutes for This
Editor's Note: This article is a reprint. It was originally published March 29, 2017.
Water pollution has many sources. Agriculture is a significant one, but clothing is another that has not received as much attention.
Nonorganic cotton contributes to environmental problems due to the fact that most of it is genetically engineered (GE) and sprayed with copious amounts of Roundup, the active ingredient in which is glyphosate, a likely human carcinogen.
In fact, nonorganic cotton is one of the most chemical-dependent crops out there. While making up only 2.4% of global cropland, it receives 10% of agricultural chemicals in total, and 25% of all insecticides.1
But synthetic fibers like polyester and nylon are equally destructive.2 In 2014, polyester — a plastic material made from crude oil — made up 60% of all fabrics produced by the textile industry.3
Unfortunately, stretchy fabrics like yoga pants and comfy, cozy fleece items have become a true bane, shedding copious amounts of microscopic plastic fibers each time they're washed. Due to their tiny size, these microfibers4 flow straight through the wastewater treatment plant without being caught.
Microfibers Account for Majority of Plastic Pollution
Testing shows synthetic microfibers make up 85% of shoreline debris worldwide,5 and are particularly concentrated in beach sediment near waste water treatment plants.6 According to estimates by the International Union for Conservation of Nature, up to 1.7 million tons of microfibers enter the ocean each and every year.7
Once in the water column, this plastic micro-debris blocks sunlight required for plankton and algae to thrive, and the ramifications of this reverberates throughout the entire food chain. To get an idea of just how severe the problem has become, consider this: In some ocean waters, plastic exceeds plankton by a factor of 6-to-1!8
Toxic dyes, fabric treatments such as flame retardants and stain resistant chemicals and laundry detergents further add to the growing environmental problems posed by clothing.
Microplastics Are a Major Issue in the Gulf
University of Florida researcher Maia McGuire, Ph.D., studies plastics in Florida waterways. At the outset, she expected to find primarily microbeads — the small plastic beads found in face and body scrubs — but she quickly realized microfibers are a far more serious concern. McGuire told the Akron Beacon Journal:9
"I totally thought we were going to be finding microbeads and [bigger] fragments. What do we do about it is the multimillion dollar question. The consensus seems to be that we need improvement in technology in washing machines and wastewater treatment plants in combination in order to try and filter out these fibers. There's just so much we don't know."
Between September 2015 and August 2016, McGuire's Florida Microplastic Awareness Project collected and analyzed water samples from 256 sites in Florida. Eighty-nine percent contained plastic, 82% of which was in the form of microfibers. Only 7% were microbeads.
As of July this year, personal care products are no longer allowed to contain microbeads.10 Beginning July 2018, microbeads will also be banned from cosmetics, and as of July 2019, they must be eliminated from over-the-counter drugs sold in the U.S. as well.11
While banning microbeads is a step in the right direction, water testing reveals they're not nearly as prevalent in the environment as microfibers are, so banning microbeads while doing nothing about microfibers is not going to have a really significant impact.
Microfibers Threaten Wildlife and End Up in Human Food Supply
It stands to reason that once these fibers are in lakes, rivers and oceans, they will be consumed by wildlife, migrating further and further up the food chain, and that is precisely what researchers have found. The fibers have been found in both table salt12 and various seafood sold for human consumption.13
Microfibers have been shown to raise mortality among water fleas14 and reduce overall food intake of crabs, worms and langoustines (aka Norway lobster),15,16 thereby threatening survival rates. Testing of both freshwater and saltwater fish show 90% have microfiber debris in their bodies.17,18
Not only do the actual fibers pose a health hazard to the sea life that consume them, since they bioaccumulate, these fibers also act like sponges, soaking up and concentrating toxins like PCBs, pesticides and oil, making the animal — which could end up on your plate — even more toxic than it normally would be.
These chemicals have been shown to cause liver damage, liver tumors and signs of endocrine disruption in fish and other seafood, including lowered fertility and immune function. Last year, citing a report19 by the British Department for Environment, Food and Rural Affairs [DEFRA], the Daily Mail wrote:20
"Microplastics have been found in a wide variety of species including zooplankton, mussels, oysters, shrimp, marine worms, fish, seals and whales. Chemicals on microplastics ingested by an organism can dissociate from plastic particles and enter body tissues …
[DEFRA] said there is evidence from animal studies that small plastic particles can cross membranes into cells, causing damage and inflammation.
Looking at the implications for humans, [DEFRA] said: 'Several studies show that microplastics are present in seafood sold for human consumption, including mussels in North Sea mussel farms and oysters from the Atlantic. The presence of marine microplastics in seafood could pose a threat to food safety.'"
According to the DEFRA report, eating six oysters could introduce about 50 plastic microbeads into your body. One-third of the fish caught in the English Channel also contain microbeads, as do 83% of scampi sold in the U.K.21
Factors That Worsen Microfiber Release
Tests show each washing of a synthetic fleece jacket releases 1.7 to 2.7 grams of microfiber.22,23,24 For perspective, a paperclip weighs about 1.5 grams.
Estimates suggest a city of 100,000 inhabitants deposit up to 240 pounds of microfibers into local waterways EACH DAY — an amount that equates to 15,000 plastic bags entering waterways on a daily basis. A number of different factors contribute to the amount of fibers shed, including:
- Age of the item — The older the fleece jacket, the more microfibers are released25
- Quality of fabric — Lower quality generic brand fleece can shed 170% more over its lifespan than higher quality fleece
- Type of fabric — In a comparison of acrylic, polyester and a polyester-cotton blend, acrylic was the worst, shedding microfibers up to four times faster than the polyester-cotton blend26,27
- Type of washing machine — While tests just a few years ago showed that top loading machines released many times more microfibers than front loading models,28 more recent high-efficiency top-loading machines now release far fewer microfibers than front loaders29
- Water temperature, length and agitation strength of the wash cycle and the type of detergent used — Heat, agitation and harsh detergents all promote the breakdown and shedding of microfibers
Potential Solutions
One of the fastest and easiest remedies is to add a filter to your washing machine that catches microfibers.30 In 2017 at one point, Wexco was the exclusive distributor of the Filtrol 160 filter,31 designed to capture nonbiodegradable fibers from your washing machine discharge.
Unfortunately, this solution only partially addresses the problem, since the microfibers will still end up in a landfill when you empty the filter into your trash can. From there, they may still enter the biological chain.
Another novel potential solution — a waterless washing machine — was developed by TERSUS Solutions in Colorado, with funding from Patagonia. It washes clothing using pressurized carbon dioxide instead of water.32 Patagonia is also looking for mitigating solutions, including product redesign to prevent the shedding of microfibers.
Perhaps the simplest way to circumvent all of these problems is also the most biologically elegant, and that is to avoid buying synthetic fiber clothing in the first place, and opt for organic cotton, hemp, silk, wool or bamboo fabrics instead.
Polyester Downfalls Beyond Microfiber Pollution
Beyond microfiber pollution, polyester and other man-made fabrics have many other environmental drawbacks, including the following:33
• Polyester is not only made from petroleum; the manufacturing process of polyester and other synthetic fabrics is also very energy-intensive, releasing large amounts of toxic air emissions, including volatile organic compounds, particulate matter and acid gases.
• Byproducts of polyester production also include water pollutants such as volatile monomers and solvents.
• Toxic chemicals are also used during the production of many fabrics, including perfluorochemicals (PFCs), phthalates, azo dyes, dimethylformamide (DMF), nonylphenol ethoxylates (NPEs), nonylphenols (NPs) and triclosan. Swedish research estimates 10% of all textile-related chemicals are potentially hazardous to human health.34
According to a Greenpeace report,35 sportswear tends to contain the highest levels of toxic chemicals, including endocrine disruptors, which may have acute toxic effects if you're susceptible. Chemicals are applied to most synthetic fabrics to improve wicking performance, provide water and/or stain resistance and decrease odors.
Some clothing manufacturers are now starting to take these issues more seriously. For example, Patagonia is working on developing textile treatments using raw, natural materials and, along with Adidas, has promised to phase out PFCs. Adidas has vowed to be 99% PFC-free as of this year. Others, such as Ibex, Alternative Apparel, SilkAthlete and Evolve Fit Wear are using organic cotton, silk blends and merino wool for their sportswear lines.36
Toxic Garment Dyes Wreak Environmental Havoc
Textile dyeing is another major environmental destroyer. Many of these facilities are located in developing countries where regulations are lax and labor costs are low.
Untreated or minimally treated wastewater is typically discharged into nearby rivers, from where it spreads into seas and oceans, traveling across the globe with the currents. An estimated 40% of textile chemicals are discharged by China.37 Indonesia is also struggling with the chemical fallout of the garment industry.
The Citarum River is now one of the most heavily polluted rivers in the world, thanks to the congregation of hundreds of textile factories along its shorelines.
Tests by Greenpeace reveal the river water contains alarming amounts of lead, mercury, arsenic, nonylphenol (an endocrine disrupting chemical) and many other toxic chemicals — all of which are dumped by textile manufacturers straight into the river without even the most basic of chemical filtration or treatments.
The final clothing items also contain nonylphenol, and it can take several washes before it's all washed out. This means the chemical is also entering your local sewer system. Nonylphenol is considered so hazardous that many European Union (EU) members have banned its use in the garment industry. It's not even allowed in imported textile goods. Notably, the U.S. has no such restrictions.
Become Part of the Solution by Cleaning Up Your Wardrobe
While some companies are actively investigating ways to produce more environmentally-friendly clothing, each and every one of us can contribute to the solution by curbing your consumption and giving more thought to what you buy and how you care for your items.
As described in my previous article on "fast fashion," the entire life cycle of a piece of clothing would ideally be taken into account before buying, as most of your discarded clothes actually end up in landfills, or are resold to developing countries where local clothing industries then suffer instead.
Most Americans have enough clothes to outfit entire villages in some other countries. There's little doubt that many would do well to absorb some of the life-affirming suggestions offered by the minimalism movement. As the director of environmental strategy for Patagonia told CBS in 2015:38
"People need to learn how to buy less and companies need to learn how to be profitable in selling less … Something has to fundamentally shift in the consumption world that reduces the pressure on the raw materials, which reduces pressure on the planet …"
To avoid toxic chemicals and reduce environmental pollution associated with the washing and wearing of clothes, consider the following recommendations:
Opt for organic cotton, hemp, silk, wool and bamboo fabrics — While such items typically cost more than nonorganic cotton and synthetics, buying fewer items will allow you to spend more on each item. On the upside, higher quality organic items tend to last far longer with proper care, so you get your money's worth in the end. |
Opt for items colored with nontoxic, natural dyes when possible — Businesses investing in organic farming and natural dyes include PACT (undergarments and loungewear), Boll & Branch (bed linens, blankets and towels), Jungmaven (organic hemp and cotton T-shirts), Industry of All Nations (clothing) and many others. |
Avoid screen printed items, as they typically contain phthalates. |
Look for the Bluesign System Certification,39 which tells you the item has been manufactured with a minimal amount of hazardous chemicals, or none. |
Avoid trademarked technical fabrics, as most are coated with chemicals that will eventually wash out. |
Be mindful of when and how you wash synthetic clothing — Wash synthetic clothing as irregularly as possible using a mild detergent. Line dry instead of putting them in the dryer. The heat and agitation will break down fibers. Handwashing or using the gentle cycle with cold water will also minimize the shedding of fibers, as will using a front loading washing machine. Avoid fabric softeners and dryer sheets. They leave a film on the fabric that blocks the wicking ability of the fiber. |
Install a microfiber filter on your washing machine. |
The Case Against Yoga Pants and Other Technical Athletic Wear
Three out of four women will have a vaginal yeast infection in their lifetime and an estimated 140 million women worldwide suffer recurrent infections.1 Recurrent infections can have a significantly detrimental impact on quality of life, and because resistance against existing treatments is on the rise, women are in dire need of viable treatment alternatives.
Most vaginal yeast infections are caused by a yeast called Candida albicans, the same fungus that is also responsible for yeast infections — also known as thrush — in the mouth, throat and gut.
The video above features an interview I did with Dr. Leon Chaitow back in 2016, in which he reviews how Candida can affect your health. Vaginal yeast infections in women is just one potential outcome.
Interestingly, according to recent research,2,3,4 zinc deficiency may be what’s allowing thrush to flourish, and this is something we did not know back in 2016. As it turns out, Candida feeds on zinc, and when zinc is low, it releases a zinc-scavenging protein called pH-regulated antigen (Pra1) to take advantage of what little zinc is available.
The problem is that Pra1 triggers inflammation in the host. The Pra1-induced inflammation is what causes the hallmark burning and itching that goes along with vaginal yeast infection.
Vaginal Zinc Cream Effectively Prevents Reinfection
In experiments, the researchers found that inflammation could be prevented in mice by manipulating genes in the yeast that blocked production of Pra1. Giving the mice a low-dose vaginal zinc gel produced the same results.
Lastly, they tested a commercially available zinc-containing vaginal cream (sold under the brand name Juvia) in six women who’d had recurring vaginal yeast infections at least once every three months. The cream was applied nightly for two weeks, and then twice a week for another 10 weeks.
At the end of the three-month study, five of the six women had not experienced reinfection. The team is now planning to conduct a larger clinical trial to confirm the effectiveness of the zinc treatment. In a media press release, research leader Duncan Wilson, Ph.D., of the University of Exeter’s MRC Centre for Medical Mycology, commented:5
“Recurring thrush can be deeply distressing and problematic, and we urgently need new treatments. Our new finding on zinc is very exciting, because it suggests that simple provision of zinc could block the production of the inflammatory Pra1 molecule, but we’re not in the position to make treatment recommendations at this stage.
We need larger scale trials to confirm the effect. Please don’t apply any products that are not designed for the genital area, as zinc can be toxic at high concentrations and it could be extremely unsafe.”
Signs and Symptoms of Candida
Candida albicans is a very pervasive yeast. Most people have it in their system, and for most, it poses no problem at all. However, if your immune system becomes disrupted from exposure to antibiotics, lack of sleep or eating too much sugar, Candida can begin to grow out of control.
One major — and clearly visible — clinical sign of Candida is a white coating on your tongue. When your microbial balance is normal, your tongue is typically clean and pink. Early intervention at this point could potentially avert many cases of thrush.
Aside from that, the symptoms of Candida overgrowth typically begins in the gut, with things like bloating, constipation or diarrhea. The normal flora in your gut produces biotin, which suppresses the ability of yeast to change into more aggressive forms.
So-called mycelial forms of yeast actually put down tiny “roots” that penetrate the mucus membrane of your gut, thereby allowing toxins from your gut to spill out and cause systemwide symptoms, such as unusual, persistent fatigue, sudden development of food sensitivities, unusual aches and pains that do not appear to have a determinable cause (such as an injury), dry skin patches, and vaginal yeast infections in women.
So, while yeast is not problematic per se — it’s a normal part of healthy gut flora — it becomes problematic when it’s not kept in check and starts to turn into the mycelial form. It’s quite likely that women who suffer recurrent vaginal infections have dysregulated gut flora, and that’s why they never experience full recovery.
How to Control Candida
To control the Candida yeast you need to starve it. This will suppress it naturally rather than using drugs to kill it outright. Candida can be viewed as a free-loader that takes advantage of your dietary and lifestyle mistakes. Things that will promote Candida overgrowth include anything that will suppress your immune function, such as:
- Eating too much refined sugar and processed foods
- Drugs such as antibiotics, steroid hormones and oral contraceptives; by changing your microbiome, they predispose Candida to grow into its more invasive form
- Lack of restorative sleep
- Lack of fresh air, physical activity and exercise
As noted by Chaitow in 2016:6
“The ... overarching approach to all these chronic problems is to ... enhance immune function, whichever way you can ... It can be just better lifestyle, better sleep, more exercise and improved, enhanced diet.
Stop feeding the yeast, stop damaging your immune function, and replenish the gut flora as best [as] possible. The yeast, controlled, takes care of itself. You don’t have to kill it … We have this natural wonderful symbiosis with our gut flora. It keeps us alive. It keeps us healthy. But if we damage it, we pay the price ...
The diet is the key. The diet needs to be as unprocessed as possible … The Mediterranean Diet is the ideal one. It’s fish (not farmed fish if possible) [and] lean meat … The agricultural industry is the main user of antibiotics [so] that’s where we’re most at risk …
Vegetables, fruits — not too much of the very sweet fruits at the beginning of the anti-Candida program, but certainly fruits like papaya are wonderful.
The avoidance of anything that is going to provoke fermentation. Sugar is key to avoid. At the beginning, that even covers things like honey in the first month or two of an anti-Candida program.
I think it’s quite a simple process. It’s healthy lifestyle, healthy diet. The program has to be coupled initially by trying to encourage more normal gut flora. We go straight into the prebiotics and probiotics. That needs to be accompanied by change in diet and avoiding antibiotics wherever possible.”
To those basic guidelines we can now add the recommendation to boost your zinc intake. Making sure you’re not zinc deficient will also help prevent Candida overgrowth in the first place. Only in severe and/or intractable cases do I recommend using an antifungal drug like Nystatin, which is a relatively benign drug with few side effects.
Useful Supplements
Chaitow recommends a number of supplements that can be useful against Candida, including:
• Caprylic acid, a medium-chain triglyceride (MCT) with eight carbons (which is why it’s also known as C8). While it’s found in coconut oil, you can also buy MCT oil, either straight C8 or in combination with capric acid (C10). No other food source converts to ketones more readily than C8, and ketones are a magnificent, efficient fuel for your body. Caprylic acid is also a potent antifungal, and Chaitow recommends it in lieu of antifungal drugs.
• Aloe vera gel contains a mucopolysaccharide with powerful immune benefits:
◦ Antifungal properties — Aloe vera contains compounds that have antifungal activities, which can help in inhibiting the growth of Candida, the yeast responsible for vaginal candidiasis. Studies have shown that aloe vera can be effective against several Candida species, including Candida albicans, which is commonly involved in vaginal yeast infections.
◦ Anti-inflammatory effects — Vaginal candidiasis can cause inflammation and irritation. Aloe vera has anti-inflammatory properties that can help reduce these symptoms. It soothes the inflamed tissues, providing relief from itching and discomfort associated with the infection.
◦ Healing properties — Aloe vera is well-known for its healing and regenerative properties. It can help in the repair of damaged tissue in the vaginal area caused by the yeast infection. This is due to the presence of glycoproteins and polysaccharides in aloe vera, which are known to aid in skin healing and regeneration.
◦ Immune-boosting effects — The immune-modulating properties of aloe vera can be beneficial in fighting off infections, including yeast infections. By boosting the body’s immune response, aloe vera can help in quicker resolution of the infection.
◦ Moisturizing effect — Aloe vera is a natural moisturizer, which can help in maintaining the natural moisture balance in the vaginal area. This is important because both excessive dryness and excessive moisture can contribute to the conditions that promote yeast overgrowth.
◦ pH balancing — Maintaining the natural pH of the vagina is crucial for its health. Aloe vera can help in maintaining the vaginal pH, thus creating an environment less conducive for the growth of Candida.
◦ Natural and gentle — Aloe vera is a natural and gentle remedy, which makes it suitable for sensitive areas like the vaginal region. It is less likely to cause irritation or adverse reactions compared to some chemical-based treatments.
How to Tell a Yeast Infection and a Urinary Tract Infection Apart
If you’re a woman, it can in some cases be difficult to tell whether you’re suffering from a vaginal yeast infection or a urinary tract infection (UTI). Both cause pain and discomfort, but there are key differences by which you can tell them apart.7
A yeast infection will produce an odorless, white, curd-like discharge from your vagina along with itching and swelling of the vagina and vulva, while cloudy, foul-smelling urine and frequent painful urination are hallmarks of a UTI.
In severe cases, a UTI can also cause fever, chills, nausea and vomiting, which typically never happens if you have a yeast infection. In rare cases, a severe UTI can also trigger acute psychosis, especially in those already suffering from major depressive disorder with psychotic features.8 It’s also known to induce delirium in elderly patients,9 and those with Alzheimer’s appear to be at increased risk.10
How to Treat UTIs
UTIs are most often caused by Escherichia coli bacteria,11 which can be introduced into your urinary tract in a number of ways, such as via your own feces or during sexual intercourse. The urethra, which carries urine out of your body from your bladder, is much shorter in women than in men, which is one reason why women tend to get more UTIs.
If not effectively treated, UTIs can progress to kidney infections, sepsis and even death. Deaths from UTIs increased by 2.4-fold from 1990 to 2019. One of the reasons for this is because many of the bacteria responsible for UTIs have developed resistance to the antibiotics used to treat them.12 According to a 2019 study,13 more than 92% of UTI-causing bacteria are now resistant to one or more commonly used antibiotics, and nearly 80% are resistant to two or more.
The good news is you don’t need antibiotics. Methylene blue is a highly effective agent against UTIs; it kills virtually any pathogen in your bladder without disrupting the microbiome the way antibiotics do. Cranberries can also be helpful. Research published in the Cochrane Database of Systematic Reviews noted that the proanthocyanidins in cranberries help prevent E. coli from sticking to the urothelial cells lining the bladder.14
How to Reduce Your Risk of UTIs
As with yeast infections, eating a diet that promotes a healthy gut flora will help reduce your risk of UTIs. Aside from that, commonsense hygiene is also important, as you want to avoid harmful bacteria from entering your urethra.
For example, make sure you wipe from front to back to prevent bacteria from entering your urethra, or better yet, install a bidet, which allows you to rinse off your genitals after each bathroom break, and pat dry. Also cleanse male and female genital areas prior to sexual intercourse.
If you’re prone to UTIs, avoid hot tubs and Jacuzzis, especially public ones, and take showers instead of baths. Also drink plenty of pure, filtered water every day, urinate when you feel the need (don't resist the urge to go) and avoid using feminine hygiene sprays, which may irritate your urethra.
Raw Poultry Responsible for Most UTIs
Lastly, use caution when handling raw poultry, as researchers have conclusively demonstrated that a majority of UTIs are caused by exposure to contaminated chicken. I reported this in “What Are the Primary Causes and Potential Complications of Urinary Tract Infections?”
In short, in most cases, the UTI-causing E. coli is introduced to your body from the food you eat, primarily concentrated animal feeding operation (CAFO) chicken, but also, potentially, pork and beef. According to one study, E. coli from food may be responsible for 640,000 UTIs in the U.S. each year, and numbers may be higher in areas near CAFOs. To avoid this risk, follow these guidelines:15
Never wash raw chicken, as it spreads bacteria around. If needed, pat the chicken with a paper towel while still in its packaging rather than rinsing it |
Place raw chicken on the lowest shelf of your refrigerator or freezer to prevent bacteria-laden juice from dripping onto other foods |
Refrigerate at 40 degrees F. or lower for no more than two days, or freeze at zero degrees F. |
Use a designated cutting board for chicken; do not cut vegetables on this board |
Thoroughly wash your hands after handling raw chicken |
Do not place the cooked meat on the same plate used to hold the raw chicken |
Cook the chicken until internal temperature reaches 165 degrees F. |
Is Zinc Deficiency Behind the Dramatic Spike in Yeast Infections?
The toxic spike protein produced in your body if you receive a COVID-19 shot is not the only health concern to be aware of. Pfizer’s mRNA COVID-19 shots also instruct cells to produce additional “off-target” proteins that could pose significant health risks.
The finding was revealed by a team of U.K. researchers1 who found a “glitch” occurred due to the way the COVID-19 shots were genetically modified. As a result, unwanted proteins are produced, with unknown effects — a phenomenon that should have been detected long before the experimental shots were given to millions of people.
Modified mRNA in COVID-19 Shots Is ‘Prone to Reading Errors’
Ribosomes decode mRNA in cells, but about 8% of the time those in COVID-19 shots may misread the coded instructions, Maryanne Demasi, Ph.D., a former medical scientist with the University of Adelaide and former reporter for ABC News in Australia, explains:2
“The researchers say that ribosomes, which are responsible for decoding the mRNA in cells, can slip and misread the coded instructions about 8% of the time — known as ‘ribosomal frameshifting.’ They say the ‘glitch’ has to do with how the mRNA in the vaccine has been genetically modified.
Unlike naturally-occurring mRNA, the mRNA that exists in the vaccines has had a ‘uridine’ base replaced with a ‘N1-methyl pseudouridine’ (to stabilize it) and unfortunately, has made it prone to reading errors.”
In May 2021, I interviewed Stephanie Seneff, Ph.D., a senior research scientist at MIT for over five decades, about the likely hazards of replacing the uracil in the RNA used in the COVID shots with synthetic methylpseudouridine.3 This process of substituting letters in the genetic code is known as codon optimization, which is known to be problematic.
At the time, Seneff predicted the shots would cause a rise in prion, autoimmune and neurodegenerative diseases and, at younger ages, blood disorders and heart failure. One of the primary reasons for this is because they genetically manipulated the RNA in the shots with synthetic methylpseudouridine, which enhances RNA stability by inhibiting its breakdown.
Now, researchers at Cambridge University and the Universities of Kent, Oxford and Liverpool, have discovered4 that the use of methylpseudouridine results in a high rate of ribosomal “frameshifting,” which causes your cells to produce off-target proteins with unknown effects. In an interview with Demasi, research scientist David Wiseman explained the concerning findings:5
“They found the Pfizer vaccine can cause your cells to make proteins that they are not supposed to make — you end up with what I call ‘Pfrankenstein proteins.’ … Imagine the following three-letter English words ABE DAN TEA TON ERA TWO — the letters are like the code on the mRNA. Now instead of starting to read the sentence at the letter ‘A’ of the first word, you frameshift to the next letter — the letter ‘B.’
That means that all the other letters are shifted to the left and it will give you a new sentence with three-letter words BED ANT EAT ONE RAT etcetera. So, the new words have a completely different meaning from the original words. This is what happened in the body of some people vaccinated with Pfizer’s product. New unwanted ‘off-target’ proteins were produced, that actually led to an ‘off-target’ immune response.”
Your Body Is Being Hijacked to Produce ‘Pfrankenstein’ Proteins
According to the study, off-target cellular immune responses occur in 25% to 33% of those who have received Pfizer’s COVID-19 shot. “It means their lymphocytes had seen the proteins before — their immune system had already been primed from a prior exposure, presumably after that person had received the mRNA vaccine,” Wiseman said.6
The study authors stated there were no adverse outcomes related to the “frameshifted products,” and the media has similarly downplayed any risk of harm. However, molecular virologist David Speicher Ph.D., told Trial Site News reporter Sonia Elijah:7
“Whenever our cells create an abundance of unintended proteins or prevent production of appropriate proteins it could lead to an unintended immune response with a huge potential to cause harm.”
Wiseman was also clear in his explanation that the “Pfrankenstein” proteins could potentially lead to health problems, including autoimmune conditions or endocrine disruption. He told Demasi:8
“What you have to realize is that your body is being hijacked, not just to produce spike protein, but also to produce other, what I call, ‘Pfrankenstein’ proteins that are completely uncharacterized. We don't know what they are, what they do, for how long they're made or how long they last in the body, and we have no idea what their toxicity is.
From the Nature paper however, we do know that these unwanted proteins elicit immune reactions in the body.
… These researchers showed that frameshifting could create chimeric proteins. Basically, as the ribosome reads the code for the spike protein, it may slip in the middle of reading the code. So, the first half is spike protein, and the second half is a Pfrankenstein protein.
Now, just imagine one half can still attach to the ACE2 receptor on cells but on the other end, you’ve got this Pfrankenstein protein dangling outside of the cells. Your immune system is going to destroy the cell because it looks foreign, and now you’ve got something that looks like an autoimmune condition.
Or you could have a protein that turns out to be not necessarily identical, but sufficiently similar to another protein in our body like a hormone and it ends up mimicking the hormone’s activity and disturbing your endocrine system.”
Reading Errors Could Be Reduced — So Why Weren’t They?
While claiming that frameshifted products weren’t harmful, the Nature study authors stated it was important for future mRNA technologies to reduce ribosome frameshifting events. They suggested that they could identify the garbled sites or sequences and alter the mRNA sequence to reduce such effects in the future.9
But as Wiseman pointed out, this should have been done already. “This work should’ve been done by the vaccine manufacturers and by the regulators before the product was authorized and given to billions of people. They’ve asked people to take a vaccine, and put it into children and they have no clue what is happening inside the body.”10
Further, the study authors are basing their assessment that there’s no risk posed by these ‘Pfrankenstein proteins’ on just 21 people. Wiseman continued to Demasi:11
“The authors wrote, ‘... there is no evidence that frameshifted products in humans generated from BNT162b2 vaccination are associated with adverse outcomes.’ But they only looked at 21 people who received Pfizer’s vaccine, so you cannot call that a serious safety study by any stretch of the imagination.
And how did they select these people? The volunteers were part of another government funded study and had not reported undue effects from vaccination. Since they did not study subjects who had reported adverse vaccine effects, the selection of participants was probably biased.
… What they’re trying to say now is that there have been no problems identified in 21 people, but in the future there may be problems, so we should just keep studying it. Are you kidding me? What they’re saying is that ‘we will inject you first and ask safety questions later.’ It’s not good enough.”
It’s worth noting that two of the researchers on the team have a pending patent application for mRNA technology,12 so they certainly have reason to downplay the problem and propose all we need to do is a bit of tweaking and all will be well moving forward.
Is Foreign DNA Integrating Into Human Cells?
Along with Pfizer's Pfrankenstein proteins, there’s potential that DNA integration from COVID-19 shots could pose a risk to the human genome. Tucker Carlson spoke with Florida Surgeon General Dr. Joseph Ladapo, who has called for an end to the use of COVID-19 mRNA shots, citing concerns about DNA fragments in the products.13
“Could foreign DNA enter your cells through the mRNA COVID vax and change your DNA — and humanity itself — forever? Sounds nutty. It's not,” Carlson tweeted. “Absolutely that could happen,” says Dr. Joseph Ladapo, the surgeon general of Florida.14 In a December 6, 2023, letter sent to the U.S. FDA and CDC, Ladapo outlined findings showing the presence of lipid nanoparticle complexes and simian virus 40 (SV40) promoter/enhancer DNA.
While there are limits on how much DNA can be in a vaccine due to concern over DNA integration, the guidelines don’t consider lipid nanoparticles and other factors in COVID-19 shots that could enhance how much DNA can enter a cell.
“Lipid nanoparticles are an efficient vehicle for delivery of the mRNA in the COVID-19 vaccines into human cells and may therefore be an equally efficient vehicle for delivering contaminant DNA into human cells. The presence of SV40 promoter/enhancer DNA may also pose a unique and heightened risk of DNA integration into human cells,” according to a news release from the Florida Department of Health (DOH).15
In a 2023 preprint study, microbiologist Kevin McKernan — a former researcher and team leader for the MIT Human Genome project16 — and colleagues assessed the nucleic acid composition of four expired vials of the Moderna and Pfizer mRNA shots. “DNA contamination that exceeds the European Medicines Agency (EMA) 330ng/mg requirement and the FDAs 10ng/dose requirements” was found.17
So, in addition to the spike protein and mRNA in COVID-19 shots, McKernan’s team discovered SV40 promoters that, for decades, have been suspected of causing cancer in humans.18 Further, according to the Florida DOH, the FDA’s own 2007 guidance states:19
- “DNA integration could theoretically impact a human’s oncogenes – the genes which can transform a healthy cell into a cancerous cell.
- DNA integration may result in chromosomal instability.
- The Guidance for Industry discusses biodistribution of DNA vaccines and how such integration could affect unintended parts of the body including blood, heart, brain, liver, kidney, bone marrow, ovaries/testes, lung, draining lymph nodes, spleen, the site of administration and subcutis at injection site.”
The FDA responded to Ladapo’s letter December 14, 2023, but provided no evidence that appropriate DNA integration assessments had been conducted. Ladapo called for a halt in their use as a result.20 “It starts at crazy but it ends at somewhere else that someone could be just so nonchalant and, frankly, willy-nilly, with something as precious and as sacred as our human DNA,” Ladapo told Carlson.21
Help for Those Suffering From COVID-19 Shot Injuries
If you’re suffering from side effects of a COVID-19 shot, your first order of business is to eliminate the spike protein — and/or any aberrant off-target protein — that your body is producing. Two remedies shown to bind to and facilitate the removal of SARS-CoV-2 spike protein are hydroxychloroquine and ivermectin. It’s unknown whether these drugs will work on off-target proteins as well, but it probably wouldn’t hurt to try.
The Front Line COVID-19 Critical Care Alliance (FLCCC) has developed a post-vaccine treatment protocol called I-RECOVER. The protocol is continuously updated as more data become available, so your best bet is to download the latest version straight from the FLCCC website at covid19criticalcare.com.22
The World Council for Health (WCH), a worldwide coalition of health-focused organizations and civil society groups, has also released a spike protein detox guide,23 which provides straightforward steps you can take to potentially lessen the effects of toxic spike protein that may be helpful. Another option is sauna therapy, which can also help eliminate toxic and misfolded proteins by stimulating autophagy.24
You've Been Genetically Hijacked to Produce Pfizer's Pfrankenstein Proteins
Fertility declines in women as they age, in part due to decreases in the quality of developing eggs, or oocytes. Little is known, however, about how this process occurs — and whether it could be prevented or slowed. A study on mice suggests it’s possible to improve oocyte quality with spermidine supplementation.1
It found that spermidine, an antiaging molecule, has the potential to reverse declining fertility in older mice, with potential ramifications for humans as well.2 Spermidine, a polyamine compound originally isolated from semen, encourages autophagy, a cellular 'self-eating' process known to positively affect aging and longevity.3
Why Spermidine Is Considered a Fountain of Youth
While spermidine was first found in semen, it has various metabolic functions in many types of cells and is naturally found in all living organisms.4 It’s also found in common foods, including aged cheese and fermented soy products, as well as mushrooms, pears and potatoes. A review published in the journal Autophagy details some of spermidine’s benefits:5
“This chemical affects numerous biological processes, including cell growth and proliferation, tissue regeneration, DNA and RNA stabilization, enzymatic modulation, and regulation of translation, among others. Furthermore, spermidine exhibits anti-inflammatory and antioxidant properties, enhances mitochondrial metabolic function and respiration, promotes chaperone activity and improves proteostasis.”
Spermidine also appears to act as a fountain of youth, offering longevity benefits in a number of species. In addition to extending lifespan, studies show spermidine offers cardio- and neuroprotection, stimulates anticancer immune response and may decrease immunosenescence6 — the gradual deterioration of your immune system — which is a leading cause of death in the elderly.7
Many of spermidine’s antiaging effects are believed to be linked to its stimulation of cytoprotective macroautophagy. According to the Autophagy review, “Age-associated conditions including cancer, neurodegeneration and cardiovascular diseases are directly connected to the intracellular accumulation of toxic debris, and its removal by autophagy constitutes a well-documented avenue for protection against age and disease.”8
In fact, spermidine’s potency is equivalent to that of rapamycin,9 a prescription immunosuppressant drug with autophagy-stimulating properties that’s used in cancer treatment.
Spermidine Boosts Fertility in Older Mice
Research published in Nature Aging suggests spermidine may have a role to play in helping fertility issues. In humans, spermidine levels decline with aging, and researchers have suggested the molecule may act as an “antiaging vitamin.”10 This may include turning back the reproductive clock.
Researchers with Nanjing Agricultural University in China found that older mice not only had less spermidine in their ovaries compared to young and middle-aged mice, but they also had more degraded oocytes and follicles. When the older mice received spermidine, however, their oocytes developed faster and with fewer defects compared to untreated mice of the same age.11
The number of follicles also increased. In humans, the number of follicles, which hold and release oocytes, is often used to measure the quantity and quality of oocytes. “Even when the researchers delivered spermidine in drinking water instead of with an injection, it still reversed signs of oocyte ageing,” according to a news release in Nature.12
And the benefits didn’t end there. The formation of blastocysts, the early stage of an embryo, also improved after spermidine exposure. Older mice given the compound also produced about double the number of young per litter compared to older mice not given spermidine.13 It’s possible that it works to boost fertility by improving mitochondrial function and helping clear away damaged cell components.
“Genes linked to cell energy production and processes that clean up cellular debris had different expression patterns in young mice, older mice and older mice that had received spermidine,” the Nature release noted. “In spermidine-enriched mice, oocytes recovered their ability to clear out broken components. The compound also seemed to enhance the function of healthy mitochondria in ageing mice.”14
What’s more, when the team applied spermidine to aged pig oocytes in a lab that were under stress, similar beneficial effects occurred, suggesting its fertility-boosting effects may apply to multiple species15 — possibly even humans. Next, the team plans to test spermidine on human oocytes in a lab.
Spermidine May Lower Mortality, Support Brain Health
Beyond offering a potential option to stave off declining fertility, spermidine is also linked to increased survival in humans. Consuming spermidine-rich food lowers mortality associated with cardiovascular diseases and cancer.16 Further, a study published in The American Journal of Clinical Nutrition found a diet rich in spermidine, at levels commonly found in the Western diet, lowers the risk of all-cause mortality:17
“Spermidine showed the strongest inverse relation with mortality among 146 nutrients studied. The reduction in mortality risk related to a diet rich in spermidine (top compared with bottom third of spermidine intake) was comparable to that associated with a 5.7-y younger age. All of the findings apply to spermidine from dietary sources and to amounts characteristically found in the Western diet …”
Cognitive benefits are also possible. In fruit flies, spermidine slows age-induced memory impairment,18 while also delaying brain aging and improving cognitive dysfunction in mice with age-related cognitive decline. Spermidine helped to decrease malondialdehyde levels, an indication of an overproduction of reactive oxygen species, while improving superoxide dismutase, which defends against oxidative stress.19
In humans, higher dietary intake of spermidine is also linked with a reduced risk of cognitive impairment.20
A research team with Manipal College of Pharmaceutical Sciences in India further suggested spermidine could be a useful therapeutic strategy for neurological disorders due to its autophagy-inducing properties. They noted that a healthy brain is dependent on its concentration of polyamines:21
“Polyamines interact with the opioid system, glutamatergic signaling and neuroinflammation in the neuronal and glial compartments. Among the polyamines, spermidine is found highest in the human brain. Age-linked fluctuations in the spermidine levels may possibly contribute to the impairments in neural network and neurogenesis.”
Protection for Your Heart and Liver, Obesity Benefits
Spermidine also offers cardioprotective properties, even when simply added to drinking water. One study on mice found feeding spermidine:22
- Enhanced cardiac autophagy, mitophagy and mitochondrial respiration
- Improved the mechano-elastic properties of cardiomyocytes, which coincided with increased titin phosphorylation and suppressed subclinical inflammation
- Preserved diastolic function
- Reduced systemic blood pressure
- Reduced cardiac hypertrophy
In humans, a diet high in spermidine is associated with reduced blood pressure and lower incidence of cardiovascular disease.23 It also reverses arterial aging, which is characterized by stiffening of large arteries and the development of arterial endothelial dysfunction, which increases the risk of cardiovascular disease (CVD).
This benefit may be due to its interactions with nitric oxide (NO) and other factors, according to researchers with the University of Colorado, Boulder:24
“Our results indicate that spermidine exerts a potent anti-aging influence on arteries by increasing NO bioavailability, reducing oxidative stress, modifying structural factors and enhancing autophagy. Spermidine may be a promising nutraceutical treatment for arterial aging and prevention of age-associated CVD.”
Research published in the journal Cancer Research also demonstrated how spermidine can be used to prevent liver fibrosis and hepatocellular carcinoma (HCC), a common type of liver cancer, in lab mice.25 Researchers noted the mice lived longer after receiving a 3 millimolar (mM) spermidine supplement in their drinking water.
The spermidine-treated mice were also less likely than their untreated counterparts to develop liver fibrosis and cancerous liver tumors, even if they were predisposed to those conditions. Whereas the mice groups treated lifelong with spermidine achieved a 25% greater life extension, those treated at older ages saw a 10% increase in longevity.
The team explained, “Consuming spermidine over the lifetime of humans provides a novel paradigm to prevent, change, or reverse the pathogenic course of liver fibrosis and HCC in a safe and cost-effective way for patients with chronic liver diseases or with high risk for developing HCC, and patients already developing HCC.”26 They further suggested that spermidine’s wide-reach health benefits may significantly impact human health for the better:
“As spermidine is a natural component … plentiful in a variety of food and agricultural products such as wheat germ, grapefruit, and Natto (a Japanese product of fermented soy), and can be chemically synthesized and developed as a drink or a dietary supplement to serve with normal diets, it will be a promising safe and cost-effective intervention that will be readily adopted for long-term intervention by the general human population to extend lifespans.”
Indeed, spermidine also alters the composition and function of gut microbiota, and intake is linked with a lower risk of obesity. The compound leads to significant weight loss and improved insulin resistance in obese mice, which may be related to alleviation of metabolic endotoxemia, which causes low-grade inflammation, and its ability to enhance intestinal barrier function.27
Spermidine-Rich Foods to Add to Your Diet
If you’re interested in harnessing spermidine’s health potential, it may be as simple as increasing spermidine-rich foods in your diet. According to The American Journal of Clinical Nutrition study:28
“Spermidine is the polyamine most readily absorbed from the human gut. A broad and diverse palette of foods contain high amounts of spermidine, such as fresh green pepper, wheat germ, cauliflower, broccoli, mushrooms, and a variety of cheeses, whereas even higher amounts are found in soybean products such as natto, shitake mushrooms, amaranth grain, and durian.”
Polyamines like spermidine are also present in aged (fermented) cheese, including blue cheese, Brie, cheddar, Swiss, Gouda, Gruyere, Manchego and Parmesan. Intake of spermidine-rich foods is important at any age but may be particularly useful as you get older, when spermidine levels tend to decline.
Can This Molecule Boost Fertility and Longevity in Aging Humans?
Editor's Note: This article is a reprint. It was originally published May 17, 2017.
You may prudently care for your skin each day, cleansing, exfoliating, moisturizing and hydrating. But, did you know that the sandwich you had at lunch may be doing more damage to your skin than skipping one of your nightly rituals?
Your skin is the largest organ in your body, responsible for temperature control, protection and excreting toxins to name just a few. Far from being an inactive covering for your internal organs, your skin is an intricate system of nerves, glands and cell layers that plays a fundamental role in your overall health and wellness.
If you want to protect your skin, age gracefully and reduce problem breakouts, it is time to care for your skin in the same way you care for your heart, control your weight and lift your mood. In other words, pay attention to the foods you eat every day.
Wheat is one of the grains in many of the processed foods at your grocery store that interferes with a healthy complexion and contributes to psoriasis and eczema outbreaks. Proteins in wheat are responsible for inflammation and changes to your gastrointestinal tract, nervous system and cardiovascular system.
Number of People With Gluten Sensitivity Rising
The extreme form of gluten sensitivity, celiac disease, affects people differently. Over 200 symptoms have been attributed to the condition. Approximately 1 in 133 people in the U.S. suffer from celiac disease1 and close to 6% suffer from gluten sensitivity.2 Dr. Alessio Fasano is the director for Celiac Research and the chief of pediatric gastroenterology and nutrition at Massachusetts General Hospital. In a Celiac Disease Foundation blog, Fasano said:3
"We also know that prevalence is rising and we're in the midst of an epidemic. Based on our study it seems that prevalence has doubled every 15 years in North America.
Why? I think it goes back to the microbiome. There are antibiotics, our diet has changed, we travel more. There have been so many changes in the past 50 years … We don't digest gluten completely, which is unlike any other protein. The immune system seems to see the gluten as a component of bacteria and deploys weapons to attack it, and creates some collateral damage we call inflammation."
In the press release announcing the publication of his book, "Gluten Freedom," Fasano said:4
"We've shown now that gluten sensitivity actually exists. It's moved from a nebulous condition that many physicians dismissed to a distinctly identifiable condition that's quite different than celiac disease. Gluten sensitivity affects six to seven times more people than celiac disease."
5 Skin Conditions Triggered by Grains
There are several different skin conditions associated with the changes that happen in your body when you eat wheat and other gluten-containing foods. Whether you have celiac disease or a gluten sensitivity, you are at higher risk for suffering these skin conditions when you eat gluten:
• Acne — This skin condition affects nearly 80% of all people between ages 11 and 30 in Western cultures.5 In contrast, the condition is virtually nonexistent in primitive societies. Hunter-gatherer communities in Paraguay were observed for three years, during which no acne on individuals were found.6
The type of symptoms from gluten sensitivity are different from celiac disease, but both include an increase in adult onset acne.7 Researchers have found a link between what you eat, how it affects your brain and your skin.8
• Atopic dermatitis — Researchers have found that atopic dermatitis is three times more likely in people with celiac disease and two times more likely in families who have members with celiac disease.9
• Psoriasis and eczema — Psoriasis is uncomfortable and sometimes disfiguring, while eczema is a term applied to a wide range of different rashes that are itchy, red and dry.
One-third of the U.S. population will experience eczema at some point in their lives. Prevalence at least doubled between 1995 and 2008. Eczema is driven in part by an allergic response and often linked to other allergic reactions, such as asthma, allergic rhinitis and acid reflux.10
Psoriasis often affects large areas of skin and is an immune reaction linked to grain proteins, namely gliadin. In a study published in the British Journal of Dermatology, participants who tested positive for antibodies to gliadin improved when they were placed on a gluten-free diet.11
The National Psoriasis Foundation also recommends those with celiac disease or a gluten sensitivity adhere to a gluten-free diet to reduce or eliminate their symptoms.12
• Recurrent aphthous stomatitis (RAS) — Although they appear similar on the surface, these mouth ulcers or canker sores are not related to cold sores caused by the herpes virus. They can be a minor annoyance or become so painful they inhibit eating and speaking.
In a paper published in BMC Gastroenterology,13 the authors propose that RAS may be the only visual symptom of gluten sensitivity and recommend patients presenting with RAS are evaluated also for celiac disease.
• Vitiligo — In this skin condition, the pigment is lost, causing white patches to appear. Although not dangerous, it can have a profound effect on an individual's life. A case report of a 22-year-old young woman with vitiligo was published in Case Reports in Dermatology.14
After previously undergoing medical therapy without success, she was placed on a gluten-free diet. Partial, but rapid repigmentation occurred in the first month and stabilized after four months of remaining gluten-free. The authors suggest that diet modifications, including a gluten-free diet, should be considered for treatment of vitiligo.
Wheat Proteins Cause Problems
You may have learned that whole grain foods are a healthy addition to your dietary plan. However, according to a growing number of experts, including Loren Cordain, Ph.D., professor at Colorado State University and an expert on Paleolithic lifestyles featured in the video above, humans are not designed to digest grains. He explains:15
"There's no human requirement for grains. That's the problem with the USDA recommendations. They think we're hardwired as a species to eat grains. You can get by just fine and meet every single nutrient requirement that humans have without eating grains. And grains are absolutely poor sources of vitamins and minerals compared to fruits and vegetables and meat and fish."
Two of the substances found in wheat responsible for many of the associated cellular problems you face are:
• Gliadin — Gliadin is the primary immunotoxic protein found in wheat gluten and is among the most damaging to your health. Gliadin gives wheat bread its doughy texture and is capable of increasing the production of the intestinal protein zonulin, which in turn opens up gaps in the normally tight junctures between intestinal cells (enterocytes).
If you suffer from celiac disease, your body will make antibodies to gliadin, resulting in damage to the delicate, absorptive surfaces of your intestines. Many people who have gluten sensitivities also experience adverse effects of the gliadin protein. This may explain why research is clearly demonstrating an increase in intestinal permeability after exposure to gliadin in those with and without celiac disease.
• Lectins — Lectins are a key mechanism plants use to protect themselves and perpetuate the plant species. They are found in highest concentration in their seed form. When animals eat foods with lectin they may experience digestive irritation; the degree of which depends upon through how many generations the animal has been eating the particular plant food.
Humans have been consuming unsprouted grains for approximately 500 generations, and we suffer more than some rodents and birds that have adapted over thousands of generations. Bread wheat has played a prominent role in lectin-induced adverse effects since it is a relatively new form and contains a wheat germ agglutinin (WGA), not eliminated through sprouting and found in higher concentrations in whole wheat.
Other Grains Act Like Wheat
If you suffer from celiac disease or have a gluten sensitivity you may want to avoid all types of gluten to reduce your potential for skin problems. There are other non-wheat grains, and even some vegetables, that have similar properties to wheat. The following foods contain chitin binding lectins that are similar in nature to wheat lectin (WGA) described above. Chitin binding lectins and wheat lectins are functionally identical and may cause similar responses in your body.
- Barley
- Potato
- Rice
- Rye
- Tomato
Gut Permeability Releases Toxins
Gluten increases the permeability of your intestinal tract, also called leaky gut. Gaps develop between the cells that make up the lining of your intestines, allowing undigested food, bacteria and metabolic waste products to leak into your blood stream. Hence, the name leaky gut syndrome. These foreign substances challenge your immune system and increase inflammation in your body.16
Research published in Gut Pathogens has theorized that an inflammatory response that starts in your gut will spread through the rest of your body and affect your skin.17 Researchers called it the gut-brain-skin connection.18
Glutinous proteins, called prolamines, increase the permeability of your intestinal tract, sensitizing your immune system and contributing to worsening acne. Leaky gut syndrome may be associated with inflammatory bowel diseases, such as Crohn's and ulcerative colitis, but even those without illness can have varying degrees of intestinal permeability.
Blood Sugar and Insulin Spikes Affect Your Skin
Wheat affects both your blood sugar levels and your release of insulin. Wheat is a carbohydrate and once metabolized increases your blood glucose levels and triggers the release of insulin and insulin-like growth factor, called IGF-1. This growth factor may increase the secretion of male hormones, such as testosterone.
The release of male hormones is not enough to trigger growth of secondary sex characteristics, such as hair or muscle growth, but may be enough to increase the secretion of sebum. This is a greasy substance on your skin that traps acne-promoting bacteria. IGF-1 may also cause skin cells known as keratinocytes to multiply, a process associated with acne.
Individuals who have an increase in intestinal permeability may also experience a release of insulin when the immune system is activated by the bacteria and protein invaders. This results in both an increase of IGF-1 and an increase in your risk of developing insulin resistance and Type 2 diabetes.19
However, it isn't only wheat that spikes your blood sugar and insulin release. I strongly recommend you consider focusing on eating a diet high in whole foods, with little to no processed foods.
A study found in the American Journal of Clinical Nutrition found young men who suffered from acne exhibited significant improvements in both acne and insulin sensitivity after eating a low-glycemic diet for 12 weeks.20 Another study demonstrated that a high glycemic diet and frequent dairy consumption are also linked to acne.21
The Paleolithic Option
Controlling acne requires a whole-body approach. Removing wheat and gluten from your diet is highly recommended to reduce inflammation and your potential for further skin damage.
Thousands of years ago, during the Paleolithic period, people were hunter-gatherers and ate primarily the meat they could hunt and plants from their environment. Missing from this ancestral diet was refined sugars, high fructose corn syrup or refined wheat products — ingredients we now know are strongly associated with insulin resistance and poor health.
It was only after the introduction of these processed foods that people began to experience the symptoms of leaky gut syndrome. Returning to a diet made almost exclusively of whole foods including organic, pastured meats and dairy products with non-genetically engineered (non-GE) plants may help you become heathier and enjoy clearer skin. As Cordain states:22
"Normalizing your system is the true strength of the so-called caveman diet. By eating foods that are concordant with your genetic ancestry, you can avoid many of the diseases associated with our modern diet.
… This genetic discordance ultimately manifests itself as various chronic illnesses, which have been dubbed 'diseases of civilization.' By severely reducing or eliminating these foods and replacing them with a more healthful cuisine, possessing nutrient qualities more in line with the foods our ancestors consumed, it is possible to improve health and reduce the risk of chronic disease."
5 Ways Grains Can Destroy Your Skin
Carnosine is a dipeptide found in meat. It’s not found in any plant foods. Dipeptide means it’s made up of two amino acids, in this case beta-alanine and histidine. The highest concentrations of carnosine are found in your muscles, brain, central nervous system1 and gastrointestinal tract,2 which gives you an indication of its potential importance.
Unfortunately, it’s also one of the top 10 most common nutrient deficiencies, especially among vegans. If you're a vegetarian or vegan, you will have lower levels of carnosine in your muscles. This is one reason why many strict vegans who do not properly compensate for this tend to have trouble building muscle.
Carnosine also binds to advanced lipoxidation endproducts (ALEs) that form from oxidized seed oils in your diet, making it a crucial aid in the detoxification of linoleic acid (LA).
Carnosine’s Physiological Roles
Carnosine has several physiological roles and benefits. For example, it:3
Provides athletic benefits — Approximately 99% of carnosine is found in muscle tissue where it facilitates lactic acid detoxification, improves muscle contraction and muscle relaxation and enhances endurance |
Alleviates diabetic nephropathy by protecting podocyte and mesangial cells4 |
Modulates energy metabolism in macrophages and microglia by restoring and/or enhancing the basal conditions |
Has antioxidant properties and scavenges reactive oxygen species (ROS) and aldehydes created by peroxidation of fatty acid cell membranes during oxidative stress5 |
Regulates the activity of stem cells |
Modulates glucose metabolism |
Enhances the degradation and/or scavenging of nitric oxide (NO) |
Promotes wound healing |
Opposes glycation6 |
Slows down the aging process by prolonging the life of cells and preserving cellular homeostasis7 |
Regulates osmotic pressure |
Modulates glutamate production and transport |
Modulates brain metabolism |
Chelates heavy metals8 |
Acts as a pH buffer9 |
Acts as a neurotransmitter |
Protects olfactory receptor neurons in the elderly |
Beef, Liposomal Carnosine and Precursors Are the Best Sources
Interestingly, a June 2023 paper10 in the medical journal Pharmaceuticals reviewed the science behind carnosine with the aim of developing new delivery systems for carnosine-based drugs. As noted in this paper:
“Because of its well-demonstrated multimodal pharmacodynamic profile, which includes anti-aggregant, antioxidant, and anti-inflammatory activities, as well as its ability to modulate the energy metabolism status in immune cells, this dipeptide has been investigated in numerous experimental models of diseases, including Alzheimer’s disease, and at a clinical level.
The main limit for the therapeutic use of carnosine is related to its rapid hydrolysis ... [This is the] reason why the development of new strategies, including the chemical modification of carnosine or its vehiculation into innovative drug delivery systems (DDS), aiming at increasing its bioavailability and/or at facilitating the site-specific transport to different tissues, is of utmost importance.”
Delivery systems currently in use or in development include intraperitoneal injections, intranasal sprays and oral administration of various nanoformulations. But while the drug industry is keen on figuring out how to profit from carnosine by making it into a drug, you certainly don’t need a drug to get these benefits.
Simply eating organic grass fed beef is one of the most efficient ways to raise your carnosine level.11 This is one of many reasons why cultured beef is not a viable substitute for real beef. Not only does fake beef lack carnosine but also B vitamins, retinol, long-chain omega-3 fatty acids, taurine, creatine and bioavailable forms of iron and zinc.12
Most carnosine supplements aren’t very effective either because the carnosine is rapidly broken down into its constituent amino acids by certain enzymes. Your body then reformulates those amino acids back to carnosine in your muscles.
An exception to this is liposomal carnosine, which appears to work quite well. Another alternative is to supplement with beta-alanine, which is the rate limiting amino acid in the formation of carnosine. According to a 2021 paper,13 daily intake of beta-alanine can raise the carnosine content of skeletal muscle by as much as 80%.
Carnosine Protects Against LA-Induced Oxidative Stress
One benefit not expounded upon in the Pharmaceuticals paper is carnosine’s ability to reduce LA-induced oxidative stress. While your body will slowly eliminate stored LA over time, provided you reduce your intake, carnosine can help reduce the oxidative damage caused by LA while your body is cleaning itself out. I take liposomal carnosine every day before meals to help detoxify LA.
The omega-6 fat LA is highly susceptible to oxidation, and as the fat oxidizes it breaks down into harmful sub-components such as ALEs and oxidized LA metabolites (OXLAMs). These ALEs and OXLAMs are what cause most of the damage.
Carnosine binds to ALEs like a magnet and acts as a sacrificial sink. It's basically a substitute target for these profoundly damaging molecules. In this way, carnosine allows your body to excrete the ALEs from your body before they damage your mitochondria, DNA or proteins. (Another molecule that protects against LA-induced damage is carbon dioxide). The illustration below shows how carnosine works in this regard.
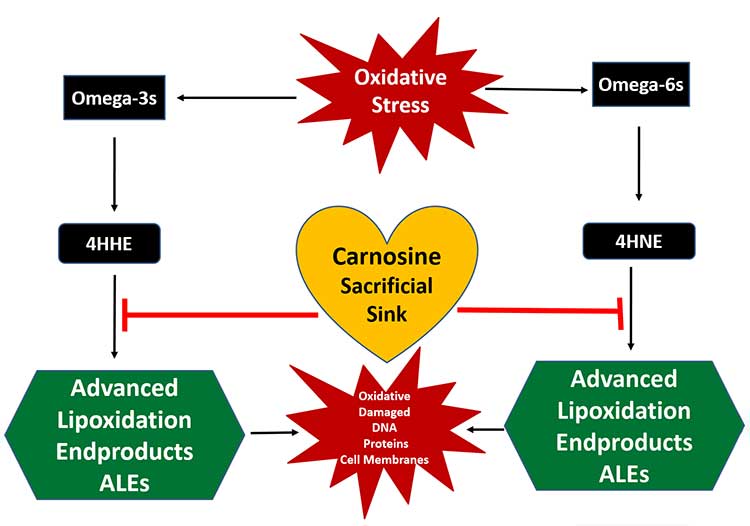
Carnosine May Be Protective Against a Wide Range of Diseases
A more detailed explanation of how carnosine protects against reactive oxygen species (ROS) and how that helps protect against oxidative stress-related pathologies is given in a 2021 paper in the journal Antioxidants:14
“A study that examined the effect of carnosine on oxidative stress in human kidney tubular epithelial (HK-2) cells indicated that carnosine decreased NADPH oxidase (NOX) 4 expression and increased total superoxide dismutase (T-SOD) activity, thus reducing the production of intracellular ROS, relieving the oxidative stress of cells, and ultimately inhibiting the mitochondrial pathway of apoptosis.
Ability of carnosine to protect against pathologies characterized by oxidative stress has been shown in a number of conditions ... Carnosine changes the reactivity of superoxide anion by forming a charge-transfer complex with the superoxide radical and also by reducing the efficiency of hydroxyl radicals, creating a compound less reactive than the hydroxyl radical.
One of the mechanisms to protect organisms from oxidative stress is the chelation of transition metals, preventing them from participating in deleterious processes involving ROS ... Interestingly, when comparing metals involved in free radical generation, carnosine was found to have a greater antioxidant activity coupled with copper than iron ...
At physiological concentrations, carnosine directly reacts with superoxide anion similar to ascorbic acid. In physiological conditions, carnosine was found to reduce oxidative damage and to improve antioxidant activity of different antioxidative enzymes ...
Experiments on aged rats showed that therapy with 250 mg/kg/carnosine per day significantly decreased oxidative stress and increased activity of antioxidative enzymes ... In similar model of aged rats, carnosine increased liver vitamin E, which further demonstrates its importance in defending the organism from free radicals.
Rising data indicate that carnosine acts as a scavenger of reactive and cytotoxic carbonyl species including 4-hydroxynonenal (HNE). HNE is an aldehyde generated endogenously by lipid peroxidation of unsaturated fatty acids that act as ‘toxic second messengers,’ extending the harmful potential of free radicals.
HNE is considered an important biomarker of oxidative stress and accumulating data indicate that it may modulate signaling pathways of cell proliferation, apoptosis, and inflammation.”
How Carnosine Protects Against Alzheimer’s
As noted in the Pharmaceuticals paper,15 one of the pathologies that carnosine is protective against is Alzheimer’s disease. In my November 2021 interview with Tucker Goodrich, he explained the role of HNE, specifically, in Alzheimer’s, and why it’s so important to get rid of it.
“In heart failure, Alzheimer’s, and AMD [age-related macular degeneration], one of the things they see is an inability of the cell to produce enough energy. The mitochondria are getting damaged. HNE does that damage. It damages 24% of the proteins in the cell, primarily around energy production.
One of the ways your cells produce energy is they basically ferment glucose into pyruvate outside of the mitochondria. This is a perfectly normal part of metabolism and they produce something called pyruvate. A molecule called pyruvate dehydrogenase takes pyruvate into the mitochondria and converts it to acetyl-CoA so the mitochondria can burn it very efficiently for fuel.
Well, one of the things HNE does is it breaks pyruvate dehydrogenase, and they see this in Alzheimer's where their cells are no longer able to produce enough energy. This is why your cells are dying in Alzheimer's.
The beta amyloid plaques in Alzheimer's disease are induced by HNE. There's a great model that came out of Harvard a couple of years ago showing that.
Even the critical, the most important part of the mitochondria, complex 5, — ADP synthase — which is what takes all the energy coming from your mitochondria and turns it into ATP, which is what fuels the rest of your body — is damaged by HNE. This is a huge issue. There's no more fundamental problem in aging and health than protein damage.”
Carnosine is the most effective scavenger of HNE, so optimizing your level can go a long way toward protecting against the HNE-induced damage that promotes Alzheimer’s.
Carnosine — A Promising Therapeutic for Obesity-Related Conditions
Elevated HNE has also been found in obese and diabetic patients,16 so there’s reason to suspect carnosine can be important in the treatment of these conditions as well. Another disease where elevated HNE plays a role is atherosclerosis. As noted in the 2021 Antioxidants paper:17
“... emerging studies have indicated that these reactive aldehydes are more than simply markers of oxidative stress.
Rather, it is suggested that these reactive species may play a significant pathogenic role in obesity-associated disorders such as insulin resistance and a carnosine analog alleviates the production or enhances the removal of reactive carbonyl species, providing promising new therapeutic compounds for cardiovascular and metabolic diseases related to obesity.”
Take Control of Your Health by Lowering Your LA Intake
As detailed in several previous articles, the evidence strongly suggests excessive LA is driving most if not all modern diseases, including heart disease and cancer. Fortunately, the solution is simple. Just lower your LA intake.
The easiest way to do this is to use an online nutritional calculator such as Cronometer to calculate your daily intake. Cronometer will tell you how much omega-6 you’re getting from your food down to the 10th of a gram, and you can assume 90% of that is LA. Anything over 10 grams is likely to cause problems. I keep my intake below 5 grams a day.
Since there’s no downside to limiting your LA, you’ll want to keep it as low as possible, which you do by avoiding high-LA foods. Keep in mind you’ll never be able to get to zero, and you wouldn’t want to do that either. You do need some LA, but since it’s found in most foods, and since you need only small amounts, there’s really no way to end up with a deficiency.
Liposomal Carnosine Is Essential for Detoxing Linoleic Acid
3.139.104.214 | United States | 508 |